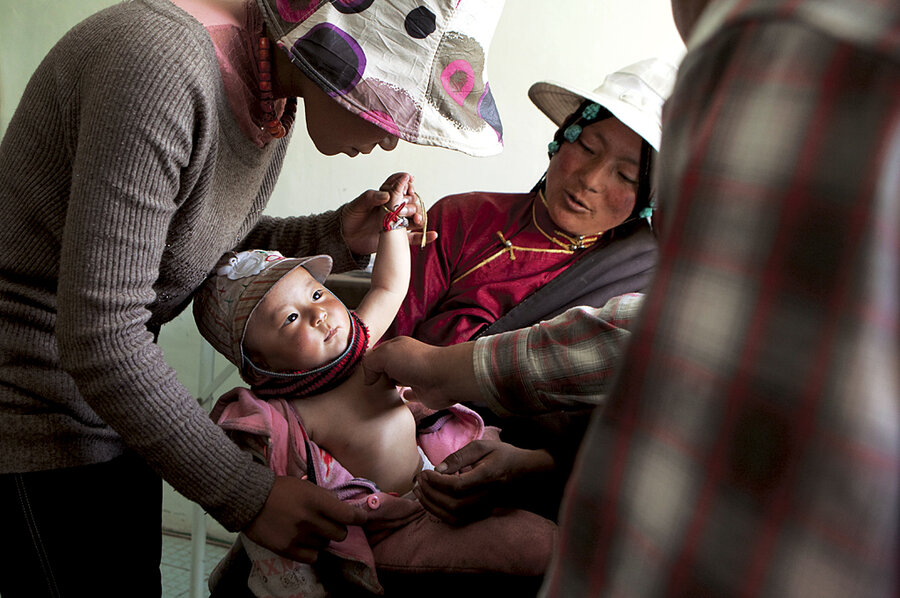
On remote Tibetan plateau, a health-care program that could be a model for China
Loading...
| Tsoke, China
When Puder, a Tibetan woman from a yak-herding family in this remote village on top of the world, had her two children, she spurned the local habit of giving birth on a bed of dried yak dung. Instead, she chose to lie on some old clothes to soak up the blood.
“I didn’t like the way I had seen other women’s babies come out all covered in dung,” says Ms. Puder, who like many Tibetans uses one name. “It seemed dirty.”
Her instinct for basic hygiene – rare among the nomadic Tibetans who graze their yak herds on these grassy slopes 12,000 feet above sea level – made Puder a natural candidate to join an innovative plan by a nearby American-funded clinic to train birthing assistants. And it is saving lives in one of China’s most isolated regions.
The Surmang Foundation’s clinic, set in a Buddhist monastery, is also pioneering a system of rural health care for the ultrapoor that some experts say could be a model for the rest of the country.
“What makes the clinic unusual is that it actually is what it should be” offering possible lessons for the government as it tries to reform its patchy and expensive health care system, says Ray Yip, a public health expert with the Gates Foundation who is advising Surmang.
Lee Weingrad, the American who set up the foundation, first came to this region in 1987 because his Buddhism teacher had once been an Abbott here.
Mr. Weingrad says he saw past the romance of saffron-robed monks spinning prayer wheels and the wild scenery to the consequences of the dire poverty that afflicts most nomadic Tibetans, many of whom live on a few cents a day.
He found that maternal and infant mortality rates in Surmang County were among the highest in the world, according to an assessment carried out by the international health experts he consulted. Twenty percent of babies were not surviving until their first birthdays, the survey reported. And 3 percent of mothers were dying in childbirth, 300 times the rate in the United States.
In response, he created the Surmang Foundation, which in 2005 began to train 40 local women like Puder as community health workers with simple, birth-related skills.
“There are so many problems in these ultrapoor areas,” says Weingrad. “We just picked out one niche where we think we can make a difference.”
Life and death
It does not take much to make a difference between life and death here.
Sometimes it might just be the slim package that the clinic’s two doctors give to expectant mothers who visit for an ultrasound exam. It contains a disposable sheet onto which the baby can be delivered cleanly and a sterile razor blade – safer than the rusty knives often used to cut umbilical cords. Sometimes it can be the presence of a woman like Puder at a difficult birth. The clinic cannot perform emergency cesareans, but she says she did once stop a woman’s bleeding with massage and Tibetan medicine. “She would have been lucky to survive had she been on her own,” Puder believes.
Sometimes it is simply a matter of knowledge. “Before, pregnant women around here paid no attention if they were vomiting or suffered swellings or bleeding,” says Drogha, the clinic’s female doctor. “They would just go on working. Now community health workers explain to them that this is abnormal and
get them to come to see me.”
At the heart of the community health worker network is the foundation’s clinic in the nearby village of Jherekhe, where Dr. Drogha and her male colleague Phuntsok offer free consultations in a simply furnished surgery room. They are trained and equipped to set broken bones and to pull teeth, (Dr. Phuntsok also cares for villagers’ Tibetan mastiffs), but most patients come with lesser ailments.
And they come in droves. Between them Drogha and Phuntsok deal with 13,000 patient visits a year, six times the load of the much better staffed government clinic 10 miles up the valley, they say.
“I used to go to a government clinic near my home but I think the treatment is better here,” says Jiucha, a yak herder, as Phuntsok takes his blood pressure. “Everyone likes this clinic,” adds his son-in-law, Gaya, waiting in the clinic’s grassy yard while his wife has an ultrasound. “The doctors are skilled and they are good people. The fact that it is free counts, too.”
Run on a shoestring budget
The clinic runs on a shoestring budget of $140,000 a year – spending one-sixth what the government clinic spends per patient, according to a 2009 study by Peking University’s Institute of Population Studies.
That is largely because the two doctors prescribe far less medicine than government-employed doctors who are paid so poorly that they make their living mainly from the markups they earn on medicines they prescribe and sell.
“When the doctors don’t profit from selling meds, that creates a tremendous amount of trust among the patients,” says Weingrad.
The profits most Chinese doctors make from such sales in government clinics and hospitals distort prescriptions nationwide, but they are a particular problem in areas such as this. “People are poor, so it is not so easy to squeeze money out of them,” says Dr. Yip, making most doctors reluctant to treat them. “Phuntsok and Drogha can treat 20 patients a day or 100 patients a day. But that doesn’t have any bearing on their salaries and nor does the amount of medicine they prescribe,” Yip adds.
“They are properly compensated and properly supported and properly supervised so they can do the work they want to and respond to local needs,” he says. “That is not happening with most rural health services across China, which are not well managed or supervised or paid.”
Surmang plans this year to introduce its health-care model, complete with networks of community health workers, to four government-run clinics in Tibetan areas.
Success, cautions Yip, will depend not only on whether the foundation can supplement the government doctors’ salaries sufficiently to compensate them for the money they will no longer earn by selling medicine, but whether the doctors can let go of their old habits of overprescribing, and whether they will accept close supervision.
“This will be difficult, but not impossible,” Yip predicts. “Creating one clinic where you control everything is one thing,” says Weingrad. “To be able to do it in the public health sphere and avail the biggest public possible of our model – that would really be something.”