AIDS: How South Africa is beating the epidemic
Loading...
| Johannesburg, South Africa
When Olga Thimbela first took in the kids, things were rosy. They were young. So was she, for that matter. She had two children of her own, and six more she was determined to raise after their mothers – one a sister and one an aunt of hers – died of AIDS, leaving the children orphaned.
Olga cleaned houses most days, and her husband, Pontsho Monamodi, worked, if irregularly, as a security guard. They brought in enough to support their expanded family, provided they were penny-wise, and they felt buoyed by knowing they were doing the right thing.
That was in 2007, a time that Olga remembers as when "things were easier, when life was simpler." It was also when the Monitor first met Olga and her family, who became part of an occasional series on South Africa's AIDS orphans. The disease has killed some 2.3 million people in South Africa, leaving roughly 1 million children without one or both parents. Only 11 percent of those were born with HIV, but all of them face challenges: depression, truancy, sexual vulnerability, and, in some cases, hunger and abuse.
Six years ago, Olga's choice was a bright spot in the bleak story of a continent beset by AIDS. South Africans were living in the worst-hit country in the worst-hit region of the world: Roughly 22.5 million had HIV, the virus that causes AIDS, in the region in 2007, according to estimates at the time by UNAIDS, the Joint United Nations Program on HIV/AIDS. That was twice the number of HIV-positive people in every country in the rest of the world combined.
For years, Thabo Mbeki, then South Africa's president, had denied that the disease even existed, and an overburdened health system, social stigma, and political sensitivities made it difficult for many patients to get tested for the disease or to get access to antiretroviral drugs. Experts, meanwhile, were predicting that the population would be decimated – that the men and women who drove the economy with their labor and consumption, who sheltered and raised the nation's children, who financially and emotionally supported their elders and parents, would be wiped out.
"That was not just a kind of ludicrous concern of some activists; that was the real prospect" – and not only in South Africa, according to Christoph Benn, spokesman for The Global Fund to Fight AIDS, Tuberculosis and Malaria, a Geneva-based nonprofit organization.
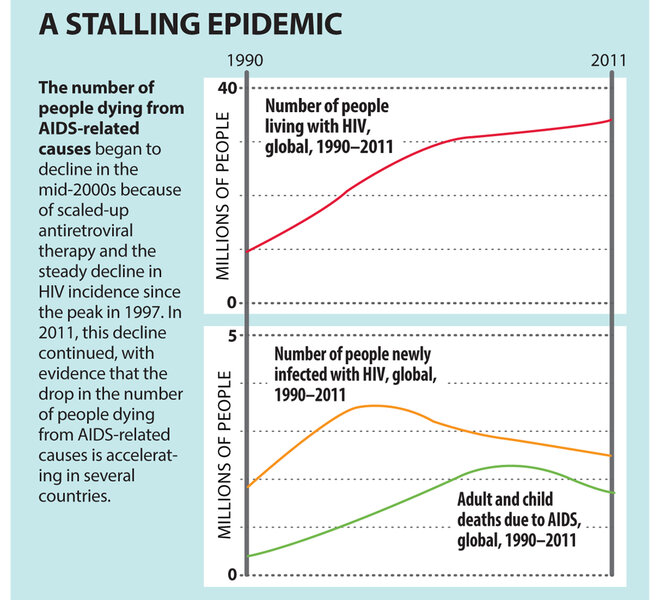
That was nearly a decade ago. Today, Africa's progress in preventing and treating AIDS exceeds even the most optimistic of earlier projections:
•The number of new HIV infections across Africa has dropped by 25 percent since 2001 – and more than 50 percent in 13 sub-Saharan African countries – according to the UNAIDS 2012 global report.
•The number of AIDS-related deaths on the continent has fallen by 32 percent since 2005, the worst year for AIDS deaths worldwide.
•Here in South Africa, progress is even sharper. Rates of infection have fallen by at least 30 percent. Nearly 2 million people are on antiretroviral drugs, known as ARVs, which have helped extend the life span of the sick and limit the transmission of the disease. Approximately 75 percent of South Africans who need ARVs have access to them, putting the country just shy of The Global Fund's 80 percent standard for universal access.
•Perhaps most meaningful to ordinary South Africans: Life expectancy in South Africa has gone up – reaching levels not seen since 1995.
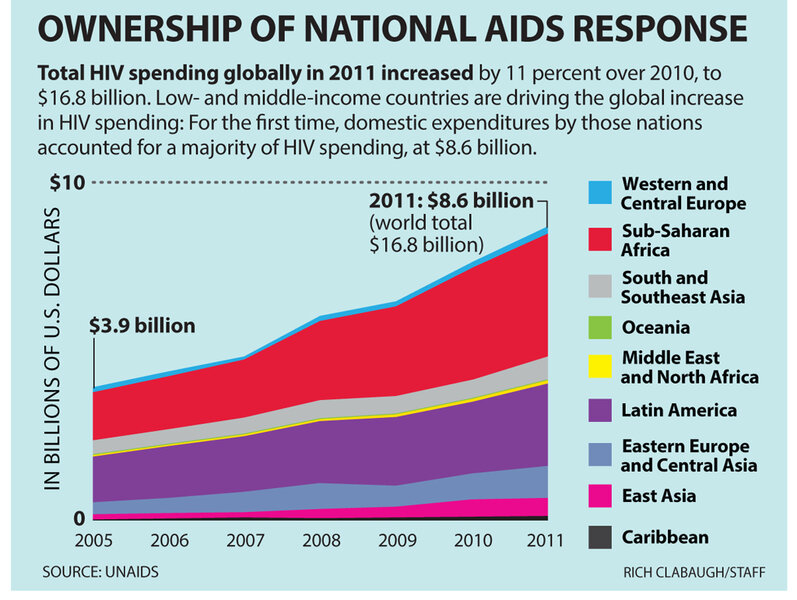
According to the US General Accountability Office, the President's Emergency Plan for AIDS Relief has spent $1.2 billion providing ARVs since 2003. Between 2008 and 2012, owing to the efforts of PEPFAR, the number of people on ARVs tripled to 5.1 million.
At the end of its second funding cycle, PEPFAR, like other international donors, is focusing on improving national capacity to manage HIV/AIDS. That management includes domestic financing streams, one burden South Africa has taken up. After years of outside assistance, more than 80 percent of the drugs its people need are paid for by the South African government itself. Last year, the South African government announced it would spend $600 million procuring ARVs in 2013 and 2014. Nevertheless, doctors and AIDS activists say supply often falls short of national demand.
But the surprising progress in beating the disease may be bringing about a shift in thinking: AIDS is no longer an acute emergency.
To be sure, it's still a serious epidemic – globally, 34 million people are living with HIV. Eastern Europe and Central Asia, where rates of new infection had been stable for several years, are seeing an increase in new infections, and infection rates in the Middle East and North Africa have increased since 2000, even as every other region in the world saw the numbers go down. And, despite remarkable progress, sub-Saharan Africa is still the region hit hardest by AIDS and accounts for 71 percent of all new infections globally.
Yet increasingly, AIDS is understood as a chronic illness, one that, health experts say, can be managed over a lifetime – a lifetime potentially as long for those living with HIV as those without.
"We can very confidently say that treatment extends the life of [HIV] patients for at least 20 years, maybe more, and [that] many of them can lead perfectly normal lives," says Mr. Benn.
AIDS takes a toll on the uninfected, too
But that's only half the story. Olga's story represents the other half – the toll that AIDS has taken, not just on the infected or ill but on South Africa and the hundreds of thousands of caregivers who stepped up to take in these orphans.
In 2006, Olga's two cousins joined her four orphaned nephews and a niece at her home, pushing the number of people living in their two-bed, four-room metal shack to 10. Yet Olga and Pontsho were optimistic, and the children seemed happy.
But things changed. By 2010, Olga's older foster children were struggling with school, first loves, and sex. The couple – and their families – were quarreling about the finances and responsibilities associated with caring for so many children. Pontsho moved out, but the couple hoped that the stresses would ease and they could restore their relationship.
That didn't happen.
Pontsho left for good; Olga – who, at age 36 now has 11 biological and foster children – doesn't hear from him anymore. Her older foster children dropped out of school and are having children of their own, children who also ultimately depend on Olga. When members of her extended family hit hard times, or simply when they've had too much to drink, they press her for money; they're convinced a modest state grant for foster parents has made Olga rich. It's far from true. Olga can't work anymore, and her boyfriend's irregular work as a taxi driver brings in a pittance.
For years, Olga had been diagnosed with a thyroid problem, which became critical during her last pregnancy. In May, her youngest child was delivered early, and she was taken into emergency surgery to fix the problem. Her doctor says having more children would be life-threatening.
There's an irony, then, in today's story of AIDS in Africa. Just as the world turns a corner, just as so many global public health statistics on AIDS finally get better, and just as patients begin living longer, the people – and they are mostly women – who stepped up in place of the dead are exhausted.
The energy and optimism they harnessed a decade or more ago when they became surrogates to a generation made vulnerable by the loss of its parents have been tried, tested, and worn down.
While the world is learning to manage AIDS, Olga and other women like her experience the disease in a different, nonmedical way. And they represent a cost of the epidemic that hasn't yet factored into most figures.
"Sometimes I think that I'm relieved the kids are growing up. Then come the [grandchildren], then come these," she says, pointing to her two youngest biological children. "I don't know if it's a gift or bad luck. I can't say it's bad luck, because children are a gift from God."
On days when even gifts from God are too much for her, she curls up on her bed and watches the American soap opera "Days of Our Lives." Sometimes that helps. Sometimes it doesn't. And sometimes, she confesses through sobs, "I feel maybe I wish I had never been born."
AIDS orphan defies the odds
It would be a mistake to misunderstand Olga's honesty. She does not seek pity, and she never evinces weakness, not even when she cries. For a woman with few friends and an absentee extended family, speaking with Monitor reporters about the challenges of her choices seems to bring a kind of relief. Her openness also reveals her as a person who takes on the weight of the world.
"I have been crying a long time. I been crying inside my heart…. I cry when I see myself, the situation that I'm in. Because I try, I try, I try so hard to give my kids a better future, a better life," laments Olga. "But it looks like I fail, you know?
"I keep asking … God, maybe I did something wrong, that's why you punish me. Why don't you let the kids alone?" she says.
Yet, her foster daughter Bulelwa Thimbela, who has a 2-year-old daughter, in so many ways has defied the odds. Her mother died of AIDS when Bulelwa was 13, but Bulelwa wasn't born with HIV, and she has Olga, who cares deeply about her. Bulelwa's pregnancy disappointed Olga: The girl was bookish as a youngster, always helping the younger children with their homework. "I thought for sure that one would have a bright future," Olga says.
But studies suggest this isn't unusual for children who lose their parents to AIDS. They are more likely than their peers to drop out of school, to suffer depression, anxiety, and abuse. They are more likely than other children, even other orphans, to be sexually active at an earlier age. They are less likely than other children to use condoms, and girls who have lost their parents to AIDS are more likely to contract HIV, and more likely to trade sex for money or material goods, even when taking factors like poverty into account.
Against this backdrop, Bulelwa is fortunate – and smart. She loved living with Olga, whose home was a place of refuge after being "abused emotionally" by another relative's family. "They used to call us names and shout at us," Bulelwa remembers. "Really I wanted to get out of there."
She felt "free and normal" in Olga's shack in Tshepisong, a township not far from Johannesburg; she devoted herself to school, and she went back as soon as she gave birth. But she dropped out again when she was briefly ill.
At 16, when Bulelwa became pregnant, she believed she and her baby's father were each other's first sexual partners (though now she suspects he may have been lying about that). Still, they used condoms, like an increasing number of South Africans, but she became pregnant after their birth control failed. Both of them went for HIV tests, which were negative.
The father of Bulelwa's baby is a lecturer at a university some distance from her home, and six months ago, when Bulelwa found out he had a string of other girlfriends, she ended their sexual relationship.
"I told him, 'We must leave this thing, because it's not going anywhere,' " she said. "If he's busy with other girls there, he's going to [get] diseases there and bring them to me."
They remain friends, and he offered to pay tuition for Bulelwa until she can secure the scholarship she lost when she dropped out of school. She'll finish her secondary degree and then specialize in business.
"I want to have my own house, to be an independent woman, and to run a business," she says. "I want to have a big house and a car."
But, she says, she does not want a husband. She lost her mother when she was only 13, and she never knew her father. Most of the adult lives she's seen have disappointed her: "Most of married women, some of them had to give up their dreams so that they could be with their families, and I don't think I will afford that kind of life. I just need to build a bright future for my baby and some of my family."
'Treatment as prevention'
Around the world, HIV-positive people, too, can dream about raising their children and improving their family's future.
Life expectancies for HIV-positive people may not be that much different than those of people without the disease, says Leigh Johnson, an epidemiologist and actuary at the University of Cape Town and a member of the International Epidemiologic Databases to Evaluate AIDS, a research consortium founded by US government health agencies.
In fact, he says, "I don't even think five years ago we would have expected to see that kind of outcome."
Treatment is doing something else few expected when antiretroviral drugs first appeared in the late 1990s: It's helping prevent the spread of AIDS. If taken regularly, ARVs reduce the presence of the virus to such low levels that an HIV-positive person essentially cannot transmit the virus to a sexual partner.
The UN is pushing for countries to adopt "treatment as prevention" strategies that would widen access to ARVs. The other key prevention measure is condoms. Between 2000 and 2008, HIV incidence dropped by 30 percent, Mr. Johnson and researchers wrote in a 2011 study – and they attributed 37 percent of that drop to condom usage. But access to ARVs has increased since the period reflected in the study. Today, ARVs and condoms, when used "under optimal conditions," are equally effective at preventing the transmission of HIV, says Ade Fakoya, senior adviser for HIV and AIDS at The Global Fund.
Drugs aren't the only prevention strategy, of course. Health workers and donors have been promoting and providing condoms to reduce the transmission of HIV for years; last year, more than one-third of funding went toward promoting "behavioral change" – getting people to have safer sex and fewer partners – and providing condoms. But in some countries, especially in Africa, condoms are still a difficult sell.
"If you use a condom, a man sometimes will feel like he hasn't even had sex," Bulelwa explains.
And UNAIDS data suggests condoms go in and out of fashion. In Cameroon, Malawi, and Nigeria, for example, the number of men reporting condom usage in their last sexual encounter has gone up in the past 10 years or so. But in Uganda, Ivory Coast, and Benin, condom usage is dropping.
Male circumcision is another prevention technique growing in popularity. Researchers say the procedure could prevent as many as 1 in 5 HIV infections, and 13 countries in South and East Africa have begun offering the procedure.
Some countries have also reported wider interventions – to curb infections among "high-risk groups" such as sex workers and men who have sex with men – although the majority of countries don't report any data on these populations at all.
UNAIDS cautions that it's impossible to say which of these interventions has had the greatest impact on reducing new HIV cases; in behavioral change programs, for instance, there are too many factors at work at the same time. There are also the usual caveats about numbers like these in general: Condom usage, for example, is a self-reported number, and researchers know that people frequently lie about their behaviors, often to match an expected norm. And then there's what Johnson calls the "natural dynamics of the epidemic."
"In any epidemic you would expect to see some kind of saturation effect, where people who are most at risk of infection get infected early on in the epidemic, and then you start to see incidence rates decline," he says.
ARVs: a new lifestyle
Over time, ARVs have become cheaper and easier to distribute. "You can now deliver those drugs in pretty simple health centers in rural areas," Benn, of The Global Fund, says. That allows health workers to "reach populations at a level we had not imagined would be possible before."
Development of generic drugs has made a major contribution to the affordability of ARVs. So, too, has the purchasing power of donors like The Global Fund and PEPFAR. Benn says that The Global Fund can buy a year's supply of ARVs for one patient for $100. (With transport, management, and administrative costs, the price of an annual supply is closer to $400.)
South African politics has changed dramatically in the past 10 years, and today the nation itself finances 82 percent of the ARVs provided to South Africans, according to Benn. That's a big change: In 2001, the government was still denying that HIV caused AIDS, and the only organization offering South Africans ARVs was Doctors Without Borders (known by its French acronym, MSF).
So if there's an emblem of this dramatic change, it's Khayelitsha, a massive township on the edge of Cape Town. Here, in 2007, MSF piloted ARV "adherence clubs," a group of no more than 30 stable HIV-positive patients who meet every two months to get weighed, pick up their medication, and discuss treatment or life challenges.
The clubs are run by laypeople – not doctors or nurses – who coordinate with pharmacists on drug delivery and keep relevant basic medical records. If patients stay stable, they only have to meet a nurse or doctor once a year, for a full checkup.
Xolelwa Xabendlini appreciates this efficiency. She works every day as a housekeeper, pulling in about $300 a month for the seven people in her household, for which she is the only breadwinner.
"We don't have to wait in this queue you see outside," she says, gesturing toward the door beyond which more than 100 people sit and wait to see a nurse and receive their ARVs. That means that Ms. Xabendlini knows she can get to her job on time, and she won't have to choose between earning a day's wage and picking up her medicine.
Other clubs meet in private homes, church halls, or public libraries. All that convenience seems to be paying off. A study published earlier this year found that 97 percent of patients in MSF's adherence clubs stayed with their treatment regimens, compared with 85 percent of those seen only in clinics. MSF's 20 adherence clubs have grown, over the past six years, to more than 600 in the Cape Town region, reaching as many as 18,000 people in a wider rollout by the provincial government.
If the idea of simplifying access and meeting patients near their homes seems almost obvious today, years ago it was revolutionary. The stigma surrounding AIDS was so corrosive that picking up AIDS drugs in the neighborhood, and thus risking recognition and public exposure, would have been unthinkable for most patients. So, too, was the idea of taking treatment out of the hands of specialists at hospitals.
Today, though, Xabendlini says, people are – and must be – more open. She talks freely with neighbors about the trips she makes to pick up her ARVs, which she's cheerfully nicknamed "chappies," after a local brand of bubble gum.
"In my street, lots of people died with HIV," she says. "If I tell them I'm also HIV positive, they think I'm lying. They see I'm strong and always laughing. I can't take this [into] my head because it would make me crazy."
Elizabeth Molomo echoes Xabendlini's optimism, and has a bit more experience behind it: She has been living with HIV for 15 years. She lives in Soweto, the largest township in Johannesburg. Every morning at 6:45, her cellphone alarm goes off, reminding her to take her ARVs. Her eldest daughter calls, too.
"I don't see myself as a sick person," she says. "I take myself as a healed person."
South Africa's AIDS success is global model
It's difficult to resist the evangelism of South Africa's good news on AIDS, and not just because there's finally relief in a country that was the worst-hit in the world for so long. It's difficult because South Africa represents what can be achieved around the world.
"The treatment scale-up [in South Africa] has been a hugely important issue," says Marcus Low of the Treatment Action Campaign. So, too, have been efforts to reduce the stigma. "It helps that the president [Jacob Zuma] publicly took an AIDS test," Mr. Low says – quite a turnaround indeed from his predecessor's denialism. The treatability of AIDS, the reduction of stigma, and awareness campaigns have contributed, too, to an increase in people being treated.
Globally, says Benn, the world has reached the point at which "we can finally defeat this disease. That means that we can really reach almost everybody."
Yet when Benn says "almost everybody," he means almost everybody who is sick. He doesn't mean Olga, or Bulelwa, or Bulelwa's toddler, none of whom have contracted HIV. But AIDS orphans and those who have taken responsibility for them bear the lifelong burden of the epidemic in a different way.
Carol Dyantyi bears the burden of AIDS, too. Ten years ago, she stumbled into a life of caring for children whose parents died of AIDS. She'd been training to be a nurse; but since 2002, she's fed, clothed, sent to school, and nurtured more than 2,000 orphans through Ikageng Itireleng AIDS Ministry, a community organization in Soweto, where Ms. Dyantyi is from. She's also watched as South Africa moved from silence on AIDS to frenzied public conversation to what she fears is another phase of silence. She's afraid South African society today has reached what she calls "AIDS fatigue."
"At the moment, it's almost like it's done.... The only time we hear [news about AIDS] is if it's World AIDS Day ... or if there's a new drug," she says. "And yet it still [exists]. It's still infringing on people's lives and causing damage."
The damage she's seen among the young people, who usually come to her program after losing their last parent and becoming responsible for their siblings, has been vast. Some end up drug or alcohol addicts. Some end up in jail. Some end up HIV positive like their parents.
Dyantyi's program tries to help all of them. She has 52 staff to help with the workload, but it's clear that Ikageng is Dyantyi. And as willing as she has been to answer her community's call for help, it's cost her, too. She's lost some donors, including PEPFAR, because of the global economic meltdown and policy shifts – and there are months when she doesn't get paid.
Divorced twice, she has four living biological children, who struggled with the time and attention she gives the orphans she cares for.
"Even though I provide [for my own family], it's almost like, 'My mom loves the [other] children more.' It gets complicated," Dyantyi says. One son committed suicide in 2010, and she is struggling to help another recover from alcoholism.
When the young people she's helped hear of Dyantyi's personal difficulties, they protest the unfairness of it.
"They said, 'No, Mom, this man can't divorce you! You can't be going through that. You can't be going through this. Everything has to be OK for you,' " she says.
Like so many teenagers, they're looking for cosmic justice. But then they realize that even Dyantyi, and the women like her who've provided a generation with surrogate love, is vulnerable.
"Yesterday, one of them said to me, 'One day you'll die. And we can't handle all of this.' "
These are the lessons Dyantyi wants to walk them through. They are lessons about more than avoiding AIDS, staying in school, or how to make macaroni. They are about making meaning out of the pain and unfairness of their young lives, about learning to make peace with a question they all, at one point or another, ask her: "Where was God when my mother passed away?"
Women like Dyantyi and Olga believe there is no answer to this question. But they also think that these kids won't find peace without another loving adult in their lives. No matter how many donors cut funds; no matter how badly the shack leaks in the cold, irrepressibly wet winters; and no matter what mistakes these kids may make themselves, someone has stepped up to love them.
And that, too, will help reclaim the future of South Africa.
• Some funding for travel for this article was provided by the International Reporting Project.