- Quick Read
- Deep Read ( 7 Min. )
Monitor Daily Podcast
- Follow us:
- Apple Podcasts
- Spotify
- RSS Feed
- Download
TODAY’S INTRO
Monitor Daily Intro for May 9, 2017
If there’s a Trump global doctrine, it may not be “America first.” Rather, it might be that a path to peace must be preceded by a show of power.
The latest evidence: Today’s news reports that President Trump is weighing plans to increase the US military presence in both Syria and Afghanistan. Sending more US soldiers to Afghanistan would be a major reversal of former President Barack Obama’s policy of withdrawal from America's longest-running war. Supporters argue Mr. Trump’s move is designed to force the Taliban into peace talks.
It might be too strong to call these steps a “doctrine,” but they are suggestive of a pattern of thought. Trump orders a cruise missile attack on Syria, he says North Korea is "looking for trouble," he threatens to cancel NAFTA, he calls NATO "obsolete" – and China a "currency manipulator." His opening salvos – rhetorical and actual – seem intended to put adversaries on uncertain footing. And then, often, a more moderate position emerges. Understanding the pattern helps reporters, and citizens, not to overreact.
Here are our five stories for today.

Help fund Monitor journalism for $11/ month
Already a subscriber? Login

Monitor journalism changes lives because we open that too-small box that most people think they live in. We believe news can and should expand a sense of identity and possibility beyond narrow conventional expectations.
Our work isn't possible without your support.
Has the US learned to thwart election meddlers?
As Washington holds hearings about Russia-sponsored hacks of the US elections, the headlines often focus on the blame game. But as the Monitor’s Peter Grier and Jack Detsch report, there’s a more fundamental problem that requires our attention: erosion of trust in America’s democratic system.
-
Jack Detsch Staff writer
The nature of Russia’s dealings with Trump campaign officials is an important question. But something that’s just as big – maybe bigger – is whether the United States can handle foreign cyber interference the next time a national election comes around. That’s a point everyone from current FBI Director James Comey to former Director of National Intelligence James Clapper has made in congressional appearances over the last week. It’s a “transcendent issue,” according to Mr. Clapper – Moscow must be happy with the divisions it’s created, so it’s sure to try again in 2018. Fighting this threat will require a unified use of American power. That means integrating hacker defense with non-techie retaliation such as sanctions. It means prosecuting cyber attackers in US courts. It means stressing information literacy to fight Russian-spread fake stories. Most of all, it means all levels of government accepting that the problem is real.
Has the US learned to thwart election meddlers?

Russia meddled in a US election in the past. Will the US be able to stop Moscow when it tries to repeat that action in the future?
That important question has been a subtext in a number of big Russia-related congressional hearings in recent days. Former acting Attorney General Sally Yates, ex-Director of National Intelligence James Clapper, and then-FBI Director James Comey (before he was abruptly fired May 9), have all testified before Senate committees this month.
Necessarily much of this public time has been spent talking about FBI investigations, the nature of ex-National Security Advisor Michael Flynn’s Russian communications, and other specifics. But at some point these current and former officials have all stopped and said that it’s important to remember the foundational problem of the hacking scandal that’s shaken American politics.
“The transcendent issue here is the Russian interference in our election process, and what that means to the erosion of the fundamental fabric of our democracy,” former DNI Clapper told the Senate Judiciary Committee on May 8. “And that to me is a huge deal. And they’re going to continue to do it. And why not? It proved successful.”
Russia’s success in sowing discord perhaps makes it harder for the US to focus on and fight the cyber intrusion that officials say stole Democratic Party emails and planted false news stories about the election. The purpose of this operation was to amplify division and turmoil in US politics. Well, mission accomplished.
As US politics is riven by partisanship like never before, and Washington fights over investigations into Russia’s connections with the Trump campaign, it seems as if the nation can’t wrap up the forensic analysis related to 2016 and unify against the threat to the 2018, and beyond.
“If we need to be focused on preventing this in the future, when are we going to get to the point where we get to do that?” says Chris Edelson, an associate professor of government at American University who specializes in presidential national security power.
The bad news is that the various probes into Russia’s attempt to manipulate the US system seem likely to stretch on for months. In the House, the Intelligence Committee investigation seems completely stalled by partisan bickering. In the Senate, a counterpart effort is plodding along, methodically. Meanwhile, the FBI is conducting its own investigation in secret.
The good news is that paralysis at the top doesn’t immobilize the entire US government. In spite of the suspected Russian influence campaign that used hacks, leaks, and fake news to undermine faith in the US political process and harm Hillary Clinton’s electability, the US has a growing menu of options to respond to digital attacks targeting the polls.
Active defense
One main approach might be called active defense. This might mean fusing intelligence, cyberdefense, sanctions, diplomacy, and other policy tools together to respond to foreign hackers.
“You may not want to respond through cyber means if you have greater pressure and leverage in other areas,” says Frank Cilluffo, director of the Center for Cyber and Homeland Security at the George Washington University and a top homeland security adviser in George W. Bush’s White House.
After all, other nations might have great cyber capabilities, but the US is a superpower that maintains unique political, military, and economic advantages. That’s helped US cyber defense in the past.
In 2015, The Washington Post reported that the US used the threat of sanctions against China before working out a deal curbing economic cyberespionage. The US had identified Beijing as the leading suspect in breaches of Office of Personnel Management databases containing 22 million government records.
In response to Russia’s 2016 election meddling, the Obama administration expelled 35 diplomats from the US, designated voting systems as critical infrastructure, and offered strong hints of covert retaliation.
“There are periods in history when new technologies make conflict offense-friendly, when it’s easier to cause harm than prevent harm,” says Nathaniel Gleicher, a former director for cybersecurity policy on the National Security Council in the Obama administration and head of cybersecurity at Illumio. “If you look throughout history, we don’t correct this imbalance by focusing more on offense – we correct it by developing a new kind of defense.”
But to actively defend against digital attacks, some lawmakers argue, there are structural problems that need to be solved, too.
The military’s top offensive hacking unit, US Cyber Command, still remains subordinate to US Strategic Command, and its leader also heads up the National Security Agency, giving it less independent authority than other US agencies with cybersecurity authorities.
Though the last Obama-era defense budget sought to give Cyber Command more independent authority, it’s not yet clear that the Trump administration will honor that pledge. Some cyber experts would like to see greater leverage to respond.
Attribution
Naming and shaming nation-state hackers that target American networks might be another aspect of defense against future electoral cyber offenses.
During the Obama administration, the Justice Department often used that approach to deter Russian, Chinese, and Iranian cyberespionage.
In 2014, the Justice Department charged five hackers associated with China’s People’s Liberation Army for allegedly breaching US companies, for instance. Last year the Justice Department charged seven Iranian hackers allegedly tied to Iran’s powerful Islamic Revolutionary Guard Corps with breaking into the computer network of a small New York dam and attacking more than 40 US companies last year.
But digital defenders aren't always up to speed on watching US networks. To better defend against national-level influence campaigns, US agencies need to have a clearer picture about what’s going on with their networks.
“They lack the rich picture of an orchestra leader bringing all of the pieces together,” says Frank Cilluffo of the Center for Cyber and Homeland Security. “The reality is technology far outpaces the ability to protect technology.”
This has led to cybersecurity experts doubting US law enforcement digital forensics in the past. Some were unconvinced by the FBI’s charge that North Korea was behind the devastating 2014 hack into the Sony Pictures network. Then Thomas Rid, a professor of security studies at King’s College London, found an encryption clue that backed up the FBI’s conclusion.
“We’re getting much better at attribution,” says Illumio’s Mr. Gleicher. “The challenge is that we have to agree as a community on what we accept – what is the proof we buy?”
After a last-minute hack of presidential candidate Emmanuel Macron’s campaign emails before French voters went to the polls on Sunday, National Security Agency Director Adm. Michael Rogers told the Senate Armed Services committee on Tuesday that the NSA tipped off French officials about malicious cyberactivity on their networks ahead of the vote.
While Admiral Rogers did not officially blame Russia, he said it appeared to be the handiwork of Russian hackers – suggesting that the US still possesses tremendous ability to track its digital adversaries as they break into and move through computer networks.
"We're watching the Russians, we're seeing them penetrate some of your infrastructure," Mr. Rogers told the committee, recalling the warnings relayed to French officials.
Diplomacy
A third part of a national cyber defense might be diplomacy. Right now, the US-Russia relationship is at a “low point,” as Secretary of State Rex Tillerson said at a press conference in Moscow last month.
But the Trump administration may have put its finger on a key aspect of deterring election hacks in the future: US-Russia diplomacy. Yet if recent history is any guide, diplomacy can have an impact on reducing digital attacks on American targets.
In 2015, the US and China signed a landmark deal to halt cyberespionage against each other’s corporations. Last summer, the cybersecurity firm FireEye reported that Chinese hacks aimed at stealing US intellectual property fell significantly after the agreement was inked.
“I just don’t think that there’s a serious effort to engage the Russians,” says Bruce McConnell, global vice president at the East-West Institute and a former deputy under secretary for cybersecurity in the Obama-era Department of Homeland Security. “It’s really a question [if] you want to work on the relationship and improve it, or whether you want to remain in a standoff, which we’re in right now.”
There’s already some precedent for US-Russia diplomacy in cyberspace.
On the international stage, the United Nations Group of Governmental Experts, a 20-country bloc led by the US, Russia, and China, has developed a set of cybersecurity “norms” that encourage members to tamp down on foreign cyberattacks, respect sovereignty in cyberspace, and steer clear of attacks on critical infrastructure.
And it appears that efforts to build upon those rules could go even further. The latest version of the Tallinn Manual, a study convened by NATO’s Cooperative Cyber Defence Centre of Excellence, aims to apply international law to digital attacks that occur when troops aren’t fighting each other on the battlefield.
“What we’re seeing in the DNC hack is that the Russians have figured out where that gray zone is and they’re operating in it,” says Exeter University professor Michael Schmitt, one of the authors of the new manual. “Now it’s up to states to clarify those gray areas.”
Part of clearing up some of the ambiguity when it comes to international conduct in cyberconflict will be defining a digital act of war. That’s something that a new Senate subcommittee, led by Sen. Mike Rounds (R) of South Dakota, plans to begin tackling later this year.
But the political situation in the US isn’t making it easier. In the movies, people are united by the appearance of a mutual adversary – the US and the USSR would come together to fight aliens, say. But that’s not happening in Washington, as President Trump continues to appear to question whether Russia was even behind the DNC hack.
Meanwhile, US spy agencies are becoming increasingly vigilant about foreign hackers aiming to sway the vote.
“What does this mean in terms of how we move ahead?” says Chris Edelson of American University.
Share this article
Link copied.

Special Report
In fight with addiction, a fraudulent ally – and a lethal result
This next story is not an easy one to read. But sometimes journalists and citizens must look hard at an evil. In a special report, the Monitor’s Warren Richey exposes a perversion of trust as young adults facing addiction seek healing. He also examines efforts to stop not just one or two crooks, but an entire system of health-care fraud.

- Quick Read
- Deep Read ( 17 Min. )
Health-care fraud in the United States, estimated at $100 billion, is more than a significant drain on critical national resources. Sometimes, it can be lethal. Two years ago, Alison Flory was searching for a way out of her drug addiction. So the young woman from Illinois enrolled in a drug-treatment program in South Florida. Thanks to the Affordable Care Act, her expenses were covered under her mother’s health-insurance policy. But unknown to her mother, Alison had been recruited from a quality treatment program into a series of shady programs engaging in lucrative insurance fraud. Rather than providing lifesaving health care, these corrupt treatment centers are warehousing addicts in fake “sober homes” so they can continue to fleece the parents’ insurance policies. In October 2016, after her mother’s insurance had been charged an estimated $750,000, Alison died of a drug overdose in the bedroom of her “sober home.” Part 1 of 2.
In fight with addiction, a fraudulent ally – and a lethal result
When she enrolled in a South Florida drug treatment program in 2015, Alison Flory had high hopes of getting her life in order and starting anew.
But instead of receiving life-saving health care, the 23-year-old from a Chicago suburb found herself being recruited from one recovery residence to another as a string of shady drug treatment facilities systematically overcharged her mother’s health insurance policy for expensive, unnecessary procedures and tests.
By October 2016, Alison was dead.
This is the story of how two troublesome national trends – booming drug addiction rates and widespread fraud in the health care industry – conspired to destroy a young woman’s life.
The US is in the midst of an epidemic of drug addiction and fatal overdoses with more than 52,000 deaths in 2015 – and the numbers are rising. The carnage is fueled in part by the widespread legal distribution of opiates to medical patients, easy availability of cheap heroin, as well as an ever-expanding lineup of other types of prescription drugs and synthetic intoxicants ripe for abuse.
The crisis is creating a broad new spectrum of Americans struggling with addiction – from suburban high school students, to young adults, to white-collar office workers, to grandmothers on Medicare.
At the same time, America is facing an epidemic of fraud in the health-care industry. Experts estimate that the government and private insurance companies lose $100 billion each year to health care scams and fraudulent claims. (That is more than the entire GDP of 131 of the world’s 195 countries. It would place 24th on the Fortune 500 list of largest US corporations, ahead of Boeing, Microsoft, and Bank of America.)
Some Americans cynically dismiss health-care fraud as something less than a major crime problem, federal investigators say. It is just money from the government or money from deep-pocket insurance companies, these cynics suggest.
But when greed replaces much needed health care for the most vulnerable in society, experts say, the result can be devastating – even fatal.
This is Alison’s story.

Over a 15-month period in 2015 and 2016, Alison moved nine times to different drug treatment centers. It was largely the work of fellow addicts – young men – who were paid to lure her and others away from their current treatment program. They did so with the promise of free rent, free use of a scooter, and other benefits – including possible romance – if the patient agreed to enroll in a particular treatment program and live in a recovery residence or sober home associated with that treatment program.
Sobriety had nothing to do with it. It is an open secret among addicts enrolled in South Florida treatment facilities that hundreds of suburban homes posing as drug-free recovery residences are little more than co-ed flop houses where the use of drugs is permitted and sometimes encouraged.
Rather than promoting health and healing, the business model that supports this multimillion-dollar health-care fraud involves warehousing addicts in fake sober homes to facilitate the perpetual fleecing their parents’ insurance policies.
Many of the addicts are complicit in the scam, using their parents’ insurance benefits like a credit card to fund a work-free and responsibility-free South Florida lifestyle while hiding behind a false façade of “treatment.”
For individuals struggling under the weight of addiction with poor judgment, low self-esteem, and inadequate coping skills, this scam and the associated lifestyle is the antithesis of rehabilitation.
“This goes beyond anything I could ever imagine, that so many people are so selfish and heartless,” Alison’s mother, Jennifer Flory, said in an interview.
At first, Ms. Flory was relieved that under the Affordable Care Act a parent’s health insurance policy extends to their children up to age 26 – including requiring open-ended coverage for drug treatment programs.
A mother of five, Flory was working in a job she didn’t particularly like, but she resolved to remain in that job because it came with a generous health insurance plan that she couldn’t otherwise afford. “I thought [having health insurance covering Alison] was a blessing. I thought, I have to keep this job until Alison is out of treatment,” she said.
Now, two years later, she has a different perspective. “Oh my God, if I would have just lost my job and not had insurance, she would still be alive.”
Evidence of fraud
Throughout her daughter’s ordeal, evidence of fraud arrived almost daily at Flory’s house in Illinois. But she didn’t know what to look for.
“I would get bills and bills and bills in the mail and half of the time I would just throw them in a drawer,” she said. “I just thought, ‘Oh cool, Alison is getting treatment.’ ”
Many of the statements were for expensive drug tests at sophisticated laboratories. Random spot tests cost $5 to $10 each and can be performed once a week or less.
In contrast, under the fraudulent business model that has taken root in South Florida and elsewhere, certain treatment programs are collecting their patient’s urine three times a week and sending it to a lab for highly sophisticated testing. Instead of $5 to $10, these tests cost anywhere from $1,000 to $4,000, or more.
Such bills are routinely being sent out and they are routinely being paid by insurance companies. They fuel an insurance-funded web of bribes and kickbacks with a steady stream of payoffs flowing between treatment centers, patient recruiters, sober homes, and laboratory operators, according to law enforcement officials.
During Alison’s 15 months in drug treatment, her mother estimates her insurance company was billed $750,000. It is not clear how much of that was actually paid by the company.
In a single day, she says, her insurance was once charged $10,000 from a treatment center that her daughter may or may not have attended for that one day. “She never told me anything about it,” Flory says.
For Flory, her daughter’s experience has produced more questions than answers.
“My question to the treatment centers is this: So you guys have billed my insurance almost $750,000 and my daughter is dead. You mean to tell me that $750,000 cannot get a person to a stable point in life to be able to function?”
How patients are recruited
Alison’s story begins with a tragedy eight years ago, in May 2009, when she was in high school. Shortly after she broke up with her boyfriend, he threw himself in front of a speeding train. Alison was at his side in the hospital when he was pronounced dead. She was 17.
The pain and guilt nearly crushed her, according to her mother. A friend wanted to help and gave her some pills to make her feel better. That is the moment the door opened to addiction.
After graduating from high school, Alison studied video-game design and art in college. Then she worked at a fabric store, as a dance instructor, and at the front desk of a hotel.
By 2015, Alison’s mother recognized that her daughter had a drug problem. Alison admitted her addiction and said she wanted her life back. She enrolled in a drug treatment program in Pompano Beach, Fla.
Once in Florida, she improved and seemed to be firmly on the path to recovery. After being released from detox, she moved to an intensive out-patient program (IOP) at a drug treatment center where she received counseling, therapy, and drug testing.
As an out-of-state patient, she needed to find a place to live during the treatment. That is where sober homes and halfway houses enter the picture. Such recovery residences are usually a group house in a suburban neighborhood shared by other recovering addicts. Legitimate recovery residences charge their patients rent and do not permit co-ed housing.
At some point during this second-level of treatment, Alison attended an anti-addiction group meeting where she was approached by an attractive young man who suggested that she move to a different treatment center and into a co-ed recovery residence where she wouldn’t have to pay any rent.
“She ended up admitting [later] that she was following him [for potential romantic reasons], but what she didn’t realize is that the guy was getting paid,” says Flory. “So it was never in her best interest, ever.”
In retrospect, it was a turning point. It took Alison off a road to recovery and put her instead on a path toward relapse after relapse after relapse.
A shady treatment center
By switching, she was leaving behind a reputable and successful treatment program to enroll in something called Reflections Treatment Center in Margate, Fla.
Reflections paid patient recruiters and brokers to identify young patients whose parents’ insurance policies could be systematically overcharged.
Scores of unscrupulous treatment centers in South Florida are conducting the same insurance scam, but law enforcement and other officials say Reflections appears to have been the worst of the worst.
Reflections was run by Kenneth “Kenny” Chatman, a convicted felon who had served time in federal prison for stealing credit card numbers. He registered Reflections in his wife’s name to conceal his own involvement.
Others in the drug-treatment community saw what he was doing.
“Everyone knows Chatman was a [problem], I mean basically we all knew,” says Richard Riccardi, owner of Fellowship Living Facilities, which runs long-established, legitimate recovery residences in Margate and Fort Lauderdale.
FBI agents raided and shut down Reflections in December. Mr. Chatman was arrested and later pleaded guilty to health-care fraud. He also admitted that he engaged in sex trafficking by recruiting some of his addicted female patients to work in the sex industry.
John Lehman, president of the Florida Association of Recovery Residences, says Chatman showed up on his radar several years ago. “All the kids that were living in various [recovery] houses in Palm Beach and Broward Counties would be transported to Reflections for ‘treatment,’ ” he says. “But none of them were getting any treatment. It was a joke.”
In 2014, Mr. Lehman began pushing for an investigation. Eventually he went to the Palm Beach Post. Reporters began writing news stories about Chatman and corruption in the drug treatment and sober home industry. The Post reported that drug treatment had become a $1 billion business in Palm Beach County, the county’s fourth-largest industry.

The stories sparked a public outcry that prompted criminal investigations. A Sober Homes Task Force was set up to identify legislative and other solutions.
But in September, just as federal agents were zeroing in on Chatman’s alleged scams, his wife, Laura, applied for a license to open a second drug treatment facility. To Lehman’s disbelief, the Florida Department of Children and Family Services granted a provisional license.
“Everyone on the planet knew that this guy should be shut down, yet they make application and are issued another provisional license,” Lehman says.
A systemic problem
It wasn’t just Chatman and Reflections. The proliferation of overbilling and sober home scams in Florida have made it difficult for legitimate recovery residences to stay in business.
There are 958 licensed drug treatment centers in Florida and roughly 3,000 legitimate recovery residences in the state. Lehman estimates that 6,000 to 7,000 houses claiming to be sober homes are really drug dens or flop houses.
At any one time there are as many as 10,000 patients enrolled in clinical drug treatment services in Florida. Of those, 75 percent are from out of state, he says.
Most will seek to live in a recovery residence in Florida rather than return home immediately after detox treatment, creating a market of addicts that is exploited by corrupt treatment centers. They pay kickbacks of $400 to $500 per week to sober homes for each insured resident who signs up for treatment, Lehman says.
The need for housing is the leverage that these treatment centers use to obtain new patients and gain access to their parents’ insurance benefits, officials say. Insurance companies will pay for drug treatment, but not forever. When the coverage lapses, the fraudsters need a way to extend the insurance gravy train.
Shady treatment centers often give their clients two options: Hit the road or “take what is behind Door No. 2,” says Lehman.
He says the option behind “Door No. 2” sounds something like this: “It says here on your medical chart you are a heroin user. You go out and have a weekend party with your friends and you shoot lots of heroin and then you go back to detox and when you get out of detox you can come back into the [IOP] program and your insurance benefits will be reset because it will be a new episode of care. And we can bill your insurance company and therefore you can have all the housing you want.”
It sets up a cycle of recovery and relapse.
“I have met people on the street and they have been down here for two or three years on the spin cycle under two or three different policies,” says Maureen Kielian, Florida director of Steered Straight, an anti-addiction group, and a member of the Sober Homes Task Force.
Ms. Kielian says there is a huge downside to drug treatment insurance scams. “It keeps those seeking recovery sick,” she says. “It just keeps them sick, and they are dying.”
Consequences: overdose deaths
Between 2012 and 2015, the number of overdose deaths more than doubled in Palm Beach County, where many of the treatment centers and recovery residences are located. The county medical examiner is still compiling the total for 2016, but the expectation is that it will almost double again from 307 to nearly 600 overdose deaths in 2016.
“It is horrific,” says Al Johnson, chief assistant in the Palm Beach State Attorney’s Office, who heads the Sober Homes Task Force.
Johnson says his office receives frequent phone calls from parents worried about their children in treatment. One said she was sure her son wouldn’t survive the year. She wanted to come to Florida to see him one last time.
Another parent called and said her daughter had relapsed and she didn’t know where she was but that she was sure she was in a “bad place.” Johnson adds: “Our investigator said, ‘Ma’am, get on an airplane, come down, get your daughter, and take her home.’ ”
The point of the task force is to save the legitimate treatment centers and recovery residences and weed out the bad actors, Johnson says. “Let’s clean up the industry so this truly is the place to go for effective, productive treatment,” he says. “There are good providers that are dedicated not to a profit motive but to recovery.”
There are signs of a potential turnaround. “I was told by the code enforcement chief in Delray Beach that 40 houses have closed down,” Johnson says, referring to flop houses.
How Reflections was shut down
One of the biggest problems faced by addicts and their family members is trying to differentiate between legitimate providers and corrupt providers.
“It’s disgusting, these people and what they do,” says Flory. “Alison’s case was particularly horrible because she got wrapped up in the Kenny Chatman thing,” she says.
“She got into every sad thing I think there was,” Flory says of her daughter’s experience in South Florida.
She partly blames herself. “I told her to trust the people who were looking over her. I told her she needs to not make decisions on her own. Let the people around her who care about her and are treating her, the doctors and so forth, let them help her to make decisions.”
The mother adds: “Little did I know I was telling her to put all her trust and faith into these people who were taking advantage of her. That’s what got me, there is so much more to it than just a young girl making bad choices.”
Among those people was Chatman.
On March 15, he appeared in federal court in West Palm Beach in handcuffs and leg irons. Prosecutors said he and his companies received fraudulent insurance reimbursement payments of between $9.5 million and $25 million.
According to a signed statement as part of his guilty plea, Chatman and others recruited some of his female patients residing in sober homes into prostitution. They advertised on websites like Craig’s List and Backpage.com.
The statement adds: “The defendant and co-conspirators provided controlled substances to these addicted patients to induce them to perform sexual acts.”
Implicit in this arrangement was Chatman’s power to also withhold controlled substances from drug-dependent women. Those who were noncompliant with Chatman’s wishes could face debilitating symptoms of sudden drug withdrawal, loss of income, and eviction from the sober home. In essence, they could be dumped on the street, sick and homeless.
By contrast, those who complied were not required to attend drug treatment sessions and submit to drug testing – but their insurance policies were billed as if they had, according to the signed statement.
At one female-only sober home, near West Palm Beach, Chatman confiscated cell phones, screwed down the windows, and prohibited the women from leaving the house, according to court documents.
Chatman could have faced up to life in prison on the sex trafficking charge, but with federal sentencing guidelines he will likely spend 12 ½ to 15 years in prison under his plea agreement. His sentencing is set for May 17.
Chatman wasn’t the only one responsible for the fraud at Reflections.
The medical director at Reflections was Donald Willems. During his tenure at Reflections, Dr. Willems was under indictment in state court on pending racketeering conspiracy charges for allegedly helping to run an opiate pill mill in Pompano Beach a few years earlier.
On March 23, Willems pleaded guilty in the Chatman case. He admitted that he used his position as a licensed physician to falsely declare that the excessive drug testing and other treatments at Reflections were medically necessary and thus covered by health insurance policies.
In addition to excessive drug tests, he authorized expensive saliva, DNA, and allergy testing, regardless of whether patients had allergies or any need for such tests.
Despite his actions in the Chatman case and the pending charges in the 2012 pill mill case, Willems’ medical license remained in good standing with a “Clear/Active” listing right up to the day of his guilty plea.
Barry Gregory, a licensed mental health counselor, worked as the clinical director at Reflections. In a YouTube video shot in September 2015, Dr. Gregory said Reflections was licensed to provide three different levels of care. “We really believe our job is to save lives and that is what we are doing,” he says on the video.
On Feb. 16, Gregory pleaded guilty to conspiring to commit health-care fraud. In a signed statement as part of his guilty plea, Gregory admitted that he knew that Chatman was telling patients that they were allowed to continue to use drugs while they were clients at the treatment center.
“As many as 90 percent of the patients [at Reflections] continued to use controlled substances while purportedly obtaining treatment,” Gregory said in the statement.
Oct. 14, 2016
In August 2016, Alison moved with her boyfriend into her last sober home, this one a yellow three-bedroom ranch-style house on NW 33rd Avenue in Lauderdale Lakes.
The neighborhood had seen better days. Two years ago, the community of 35,000 was named one of the 10 most dangerous towns in Florida. Crack cocaine was being sold in the parking lot of a convenience store a few blocks from the sober home.
But Alison had a reason to move in. She could live there rent-free, and was also being paid $350 a week. According to her mother, the payment was for her work as a “house manager.” She was also enrolled at Reflections and supposedly was attending treatment sessions three times a week. This was her second stint as a patient at Reflections.
Flory confirms that her insurance was being billed during that period for treatments and drug tests.
The sober home on NW 33rd Avenue was rented by a man who lived next door and ran the sober home. He had a van and would transport the clients to their treatment sessions at Reflections. According to Alison’s mother, sometimes Chatman himself would arrive in a van to pick up Reflections clients.
At some point in the early morning hours of Oct. 14, Alison and one of her housemates, Nicole De La Pena, decided to smoke crack cocaine. Earlier, they made a purchase down the street, according to an account Nicole gave to her mother, Johanna.
What neither Alison nor Nicole could know was that the crack cocaine they were about to smoke was laced with carfentanil.
Three weeks earlier, the Drug Enforcement Administration had issued a nationwide warning about carfentanil, a synthetic opiate said to be 10,000 times more powerful than morphine. The DEA warned that mere skin contact could cause an overdose in a paramedic or police officer responding to an emergency. A dose of carfentanil about the size of a grain of salt would likely be fatal to a human, experts say.
Alison was last seen alive by her boyfriend at 4 a.m. when he saw her asleep in her bed and still breathing.
Later that morning around 8:30 a.m., the man who ran the sober home arrived to take clients to their treatment sessions at Reflections. He was unable to awaken Alison.
According to a recording of the 911 call, it took the house manager 37 seconds to vocalize a muffled, “Hello.”
“Your phone dialed 911. Do you have an emergency,” the operator asked.
“Yes, I am trying to figure out right now,” the manager responded. “Um, um, I have, I have, I have someone in here and she’s – we’re trying to wake her up but I don’t feel no pulse.”
At no point during the 911 call was the manager able to state the address of his sober home or even the nature of the emergency despite requests from the emergency operator. The call lasted one minute and 48 seconds.
Some advocates for reform of the sober home industry say that those who run sober homes should be trained in CPR and maintain a stock of naloxone, an antidote for opiate overdoses.
It is not clear that this would have saved Alison’s life on the morning of Oct. 14, but experts say it might have.
When paramedics arrived, they were unable to revive Alison. She was pronounced dead at 9:08 a.m.
The medical examiner’s report says Alison died of carfentanil and cocaine toxicity.
Police photos taken inside Alison’s room in the sober home shortly after her death show the presence of three postage-stamp sized pink plastic bags with white residue inside. Two were on the floor near her closet, one was inside a shoe. They are the type of bags that are used to sell street quantities of illegal drugs.
In addition, the photos reveal a five-inch glass tube with smoke residue inside and seven pills in a cluster on the night stand beside the bed.
'All they care about is the money'
Flory says there is no way to measure the pain caused to parents and other family members of addicts lost to drug addiction. “It is the most horrible thing I would imagine ever having to go through, losing my oldest kid,” Flory says.
“We talked, we confided in each other, we hung out, we had the same sense of humor,” she says of her daughter. “She was literally my best friend.”
Until Alison’s experience in South Florida, Flory said she never really considered the full cost of fraud in the American health-care system.
“I just thought it didn’t really affect anybody. Yeah, insurance fraud is making people’s premiums go up, but that’s it,” Flory says. “I didn’t know it was killing people.”
At some point during her ordeal in the South Florida spin cycle, Alison apparently figured it out. In a moment of candor she told her mother it was fraud, that it was all a gigantic scam. “All they care about is the money,” Alison said, according to her mother.
“I told her, no, that’s not true,” Flory said she replied to her daughter. “She told me that these people are just greedy and selfish and they just want to make money. I said that is ridiculous.”
The mother adds: “I just thought she was trying to be dramatic. But yeah, she is laughing now. She is looking down and saying, ‘I told you so.’ ”
Flory says she is telling Alison’s story for one reason – to save other lives.
“The most important thing is to understand what is happening and put an end to it,” she says. “To find a solution so that other people don’t have to go through this.”
- Tomorrow, in part two of our special report, we’ll look at how mothers of drug addicts are creating an informal network to help others avoid the pitfalls they experienced.
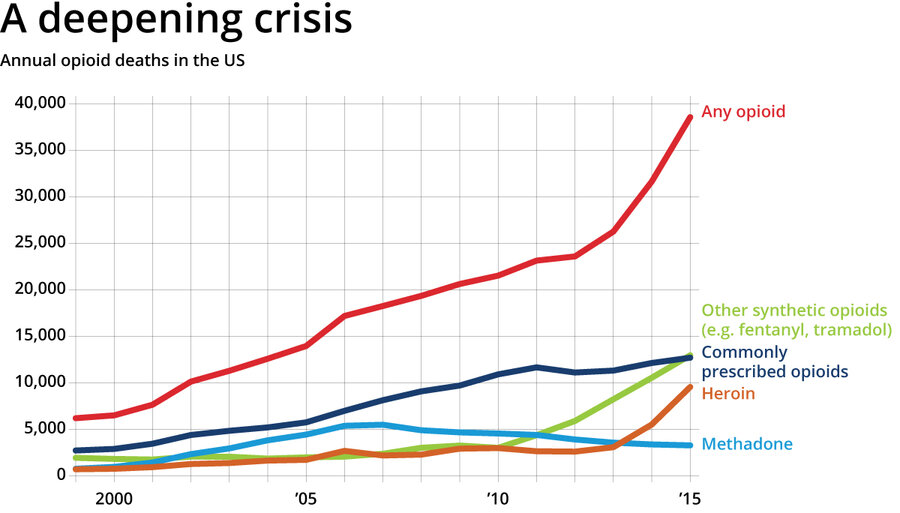
US Centers for Disease Control

Why South Korea looks poised to keep trying with North
A son of North Korean refugees, the newly elected leader of South Korea sees cooperation with the North as a way to prevent war. But that particular path to progress could clash with the Trump administration’s tougher approach. Or perhaps it's a case of good cop, bad cop.

- Quick Read
- Deep Read ( 6 Min. )
South Korean President-elect Moon Jae-in has proposed more engagement with North Korea. To his supporters, that may be just one policy plank. But it holds an outsize importance for South Korea’s decades-old alliance with the United States, which is pushing a distinctly harsher strategy to rein in the regime of Kim Jong-un. That’s not to say voters in the South went to the polls determined to usher in an administration friendlier to the North. In one preelection survey, just 18.5 percent of respondents called “national security and liberal democracy” their top concern. More of them named tackling corruption or focusing on the economy. Mr. Moon’s mandate likely has more to do with public antipathy toward conservative politicians after ex-President Park Geun-hye’s scandal-ridden tenure than warmer attitudes toward the North. And his calls for engagement face plenty of opposition at home, as well.
Why South Korea looks poised to keep trying with North

As the United States ratchets up pressure on North Korea over its accelerating missile and nuclear tests, South Korea has cast an emphatic vote for rapprochement with its isolated neighbor, electing its first pro-engagement president in nearly a decade.
Moon Jae-in, a former human rights lawyer and democracy activist, declared victory late Tuesday evening after his two main rivals conceded the election. Early Wednesday morning, with 80 percent of votes counted, Mr. Moon held the lead with about 40 percent of votes, according to the National Election Commission. The winner's dovish approach may put him at odds with US President Donald Trump’s policy of squeezing Pyongyang through sanctions and the threat of military force.
That's not to say voters went to the polls determined to usher in an administration with friendlier views toward the North. In an opinion survey by RealMeter carried out before the election, just 18.5 percent of respondents said "national security and liberal democracy" was their top concern in selecting a candidate, while 27.5 percent named tackling corruption their first priority, and 24.5 percent named the economy. Mr. Moon's mandate likely has more to do with public antipathy toward conservative politicians after ex-President Park Geun-hye's scandal-ridden tenure than warmer attitudes towards the North, and his calls for engagement face plenty of opposition at home, as well.
But no matter where North Korea ranks on most South Korean voters' priorities, the winner's more conciliatory policies, with Seoul calling more of the shots, will likely complicate its longstanding alliance with Washington.
“President Trump is more interested in leveraging China to stop North Korea's nuclear ambition, and, if found ineffective, the second phase is putting maximum pressure on Pyongyang with military power to draw Kim Jong-un to an advantageous negotiation table,” says Nam Chang-hee, an international relations professor at Inha University in Incheon, a port city about 20 miles west of Seoul. “In case a Moon administration fails to coordinate accordingly with the Trump policy, the alliance might go through difficult challenges.”
South Korea has been one of Washington’s closest allies since the 1950-1953 Korean War, during which they fought North Korea to an enduring stalemate, and currently hosts 28,500 US troops on its soil.
Reconsidering 'sunshine'
Moon, who replaces Ms. Park following her impeachment over a far-reaching corruption scandal, has floated a revival of the “sunshine policy” implemented by Nobel Peace Prize-winning President Kim Dae-jung and his successor, Roh Moo-hyun, the country's last liberal president and Moon's former boss.
The president-elect, who was the late Roh’s chief of staff and a top aide, sees diplomacy and economic cooperation as a means to reduce cross-border tensions, induce Pyongyang to abandon its weapons programs and, ultimately, pave the way to Korean reunification.
“There will be a paradigmatic change from a policy of pressure and sanctions to that of engagement,” says Chung-in Moon, who served as a top advisor to the Kim and Roh administrations, which governed between 1998 and 2008. “The Moon government will make every effort to improve ties with North Korea.”
While supporting sanctions as one tool to rein in Pyongyang, the new occupant of Seoul’s Blue House has pledged to restart the Kaesong Industrial Zone, a jointly operated industrial park situated just north of the border, and sightseeing tours to a scenic North Korean mountain, both of which were shut down by recent conservative administrations. If implemented, Moon’s proposals could leave him open to charges of undermining US and UN sanctions designed to punish the regime, especially as Washington lobbies nations to cut off economic and diplomatic relations with Pyongyang.
Moon, the son of refugees who fled North Korea during the war, has also offered to meet Kim Jong-un, the Pyongyang strongman, under the right conditions, although Trump has expressed similar intentions. Presidents Roh and Kim both met with second-generation dictator Kim Jong-il.
Seoul in the driver's seat
“I do not see it as desirable for South Korea to take the back seat and watch discussions between the US and China,” Moon said in an interview with The Washington Post last week, outlining his belief that Seoul should take the lead on issues affecting the Korean Peninsula. “I believe South Korea taking the initiative would eventually strengthen our bilateral alliance with the US.”
While acknowledging the importance of the US-Korea alliance, Moon has repeatedly argued for the South to assert greater independence from Washington, echoing his mentor, Roh, who won office in 2002 during a nadir in US relations, having pledged to be the first leader not to “kowtow to the Americans.”
Prior to his election, Moon criticized the deployment on Korean soil of THAAD, an American missile defense system, arguing that its implementation was rushed to deprive the incoming administration of the chance to consider its merits. Many South Koreans are opposed to the defense system, citing concerns about China and Russia's opposition to it. In an opinion poll carried out by the Asan Institute for Policy Studies in March, 38 percent of South Koreans said they disapproved of the missile shield, with 51 percent in favor.
Compounding the controversy, Trump enraged many Koreans by suggesting last month that Seoul should foot the bill for the $1 billion system, although the administration quickly reaffirmed its commitment to paying for it. Trump's suggestion was the latest of several White House moves that alarmed Seoul. In mid-April, the president's comment that "Korea actually used to be a part of China" – made as he described his recent meeting with Chinese leader Xi Jinping – outraged South Koreans. The following week, when it was revealed that the "armada" Trump had said was on its way to Korean waters, the USS Carl Vinson, was actually sailing in the other direction at the time (although it has now arrived), some South Koreans were left doubting the US's commitment to their security.
“What [President Donald Trump] said was very important for the national security of South Korea. If that was a lie, then during Trump’s term, South Korea will not trust whatever Trump says,” South Korean presidential candidate Hong Joon-pyo, who came in a distant second to Moon, according to Tuesday evening exit polls, told The Wall Street Journal.
A return to the past?
But Moon will also have to reckon with engagement's controversial legacy here, especially among conservative South Koreans. Pyongyang tested its first nuclear weapon in 2006, despite the extensive efforts of the Roh and Kim liberal administrations to improve ties, including providing the North with some $4.5 billion in aid.
Since then, the Kim regime has carried out four more nuclear tests, and is expected to carry out its sixth soon.
In 2010, just days before the North shelled a South Korean island, killing four, Seoul’s Unification Ministry released a report arguing that a decade of engagement had induced “no positive changes” in Pyongyang’s behavior toward its neighbor or its own people. In a poll carried out by the Asan Institute of Policy Studies in March, South Koreans gave North Korea a favorability score of just over 2 when asked to place the country on a scale of 1-10.
“Many people are indignant about a return to the past because the money the South gave to North Korea became weapons for killing South Koreans,” says Song Dae-sung, a national security analyst and former brigadier general in the Korean Air Force.
“Moon Jae-in and the supporters of ‘sunshine’ think of South Koreans and North Korea as one people, and believe North Korea’s feelings of fraternity will stop it from ever using weapons of mass destruction on the South. But this is not the truth,” Song adds.
For now, Moon's popularity likely has more to do with antipathy toward Park and her party than enthusiasm for his North Korea policies, according to Dr. Nam, the international relations professor. But, he says, the public could warm up to engagement in the likely scenario that under Moon, “Pyongyang will tone down their hostile stance toward Seoul, expecting leeway from beefed-up international pressure and sanctions.”
Dr. Moon, the former presidential advisor, acknowledges that South Korea’s new president is likely to face major obstacles to his agenda, from US policy and domestic opinion to North Korean provocations. Still, he believes it’s time for South Korea to take a “proactive role in bringing peace on the Korean Peninsula.”
“The sunshine policy deserves another try,” he says.

What US-Kurdish alliance means for ISIS fight, and for Kurds
US soldiers are working closely with the Kurdish fighters in the battle against ISIS. But here’s the rub: Turkey, another US ally, is bombing the Kurds. One question we considered: What are the moral obligations of this US alliance?
- Quick Read
- Deep Read ( 7 Min. )
With American help, the Kurdish YPG have become the only US-allied fighters in Syria capable of knocking the Islamic State (ISIS) out of its self-declared capital, Raqqa. They are not the first Kurds to have helped the United States achieve its military goals against ISIS. In Iraq, the fierce peshmerga have been instrumental. And ISIS is just the latest enemy that the US and Kurds have faced together. But often the Kurds have come to see these joint ventures as leading to betrayal. Among their most bitter memories: the 1991 uprising against Saddam Hussein that the US encouraged but allowed to be crushed. So what do the Syrian Kurds expect in return for their sacrifice? Support for a de facto autonomous zone in Syria. And that puts them squarely at odds with Turkey, a NATO ally of the US. That leads to an uncomfortable truth: Despite the current US support, Syria’s Kurds risk being abandoned once the anti-ISIS operations are over and Turkey demands that the US choose between its allies.
What US-Kurdish alliance means for ISIS fight, and for Kurds

The symbolism of American solidarity with its problematic but highly valued Kurdish allies could not have been more potent.
With American flag patches affixed to the chests of their uniforms, US military officers attended the funerals last week of Syrian Kurdish fighters of the People’s Protection Units (YPG), pivotal US allies in the fight against the so-called Islamic State (ISIS) in Syria.
The Kurdish fighters had been killed in airstrikes by another US ally, NATO member Turkey, which considers the YPG to be terrorists.
That wasn’t the only American flag-waving on behalf of the YPG: To deter further Turkish attacks, convoys of US armored vehicles flying the stars and stripes snaked along Syria’s northern border with Turkey, creating a human buffer to protect a local fighting force that the Pentagon has invested in for more than 2-1/2 years, despite constant Turkish complaints.
“I’ll tell you, it was like a wedding was going on,” Ivan Abu Zeid, a resident of Qamishli town, told Syria Direct website about the US arrival. “People were thrilled, clapping and waving at the American soldiers.”
With the US help, Syrian Kurds have become the only local fighters capable of knocking ISIS out of Raqqa, the capital of its self-declared caliphate, and are advancing to do so at America’s behest.
And they are not the first Kurdish force to have helped the United States achieve its military goals against ISIS in the region. In Iraq, the peshmerga were instrumental both in containing the breathtaking advance of ISIS in 2014 and, since then, in rolling them back, including the fight that has cornered ISIS in its last urban toehold in northwestern Mosul.
The fight against ISIS is just the latest instance in which the US and Kurdish fighters have joined forces. At times, US and Kurdish interests have coincided. At others, they’ve been complementary.
Yet often, from the Kurds’ perspective, these joint ventures came to be defined by betrayal. Among their most bitter memories: the 1991 Kurdish uprising against Saddam Hussein that the US encouraged but allowed to be crushed.
The Kurds' gamble
The Kurdish experience with America raises the question: How strong is the US-Kurdish alliance this time? What do the Syrian Kurds expect in return for their sacrifice? And, despite the optics of current US military support, do Syria’s Kurds risk being abandoned once the anti-ISIS operations are over and Turkey demands that the US choose between its allies?
“This is a big risk that the YPG and PYD have been taking,” says Noah Bonsey, a senior Middle East analyst for the International Crisis Group (ICG), using the acronym PYD for the Syrian Kurds’ political arm, the Democratic Union Party.
“Their gamble all along has been that working with the US will not only steadily expand their territorial holdings and gradually increase their international political legitimacy, but indeed it will deter Turkish attack,” says Mr. Bonsey.
Yet the Turkish airstrikes on April 25, which killed 20 YPG fighters in northern Syria and struck northern Iraq, were a surprise wake-up call that US and Russian influence over Ankara may be limited – and that Turkey, if it chooses, could be a spoiler to the Raqqa offensive. Already, US and YPG deployments in Syria have been altered to defend against Turkish attack instead of focusing solely on the Raqqa offensive.

Here's why the YPG is a problematic US ally: While its fighters command and lead the 50,000-strong umbrella Syrian Democratic Forces (SDF), which include some Arab and other units, it is also the Syrian affiliate of the Kurdistan Workers’ Party (PKK), which has conducted a decades-long insurgency against the Turkish state that has flared anew since mid-2015.
The PKK is officially considered a terrorist group by the US and Europe, as well as by Turkey. And the backbone of YPG leadership are PKK cadres, often with years of fighting experience.
What the YPG wants
In its approach to Raqqa, the White House has expanded a YPG-centered plan inherited from the Obama administration. In March, President Trump added 400 US Marines to the 300 Special Operations Forces already assisting the SDF in northeast Syria. And May 8, according to NBC News, the White House authorized the transfer to the YPG of infantry arms and ammunition and engineering breaching equipment such as bulldozers.
But Turkey’s President Recep Tayyip Erdoğan, when he meets Mr. Trump May 16, will insist again that the US stop working with the Syrian Kurds and embrace a Turkish plan to use non-Kurdish forces in the Raqqa offensive.
Wading through the confusing jumble of acronyms, US officials carefully distinguish between the PKK and their YPG allies. But Mr. Erdoğan last week again compared the YPG to ISIS and Al Qaeda, saying “they are all the same,” and that it was a "common responsibility to eradicate those terrorist organizations.”
Turkey was “seriously concerned to see US flags in a convoy that has YPG rags on it,” Erdoğan said earlier, adding he would raise the issue with Trump.
Syrian Kurds reject the terrorist label, and the YPG counted 67 Turkish attacks on its positions in April. In turn, it said it destroyed Turkish tanks and armored vehicles.
“We will not give in to Turkey’s attempts to drag us into conflict because our goal is to fight terrorist organizations … and liberate the areas that [ISIS] control,” SDF spokesman Talal Silo told the AraNews website, saying the group expected that the US presence would prevent Turkish attacks.
The result is a careful balancing act for the White House, as it prioritizes forcing ISIS out of Raqqa over ties with a strategic ally. But it also raises questions about what Washington can deliver in return to the Kurds.
“You are hitting Raqqa, not because Raqqa is a Kurdish town – it isn’t – but because the US is asking you to do it. They are going to shed blood in the expectation of something,” says Bulent Aliriza, director of the Turkey Project at the Center for Strategic and International Studies (CSIS) in Washington.
The YPG expectation will be for support for a de facto autonomous zone, he says, similar to that set up for Iraqi Kurds in 1991 in northern Iraq. Such a zone was included in one unofficial paper circulated last week by Russia during Syria peace talks in Astana, Kazakhstan. But the final agreement – signed by Russia, Iran and Turkey on Thursday – to set up four areas it called “de-escalation” zones made no provision for the Kurdish region of northeast Syria.
For Turkey, an unacceptable threat
Turkey has refused such an outcome, stating that a Kurdish entity along its southern border would present an unacceptable opening for the PKK to launch attacks. But that is not the prism through which much of the anti-ISIS coalition is looking, which complicates Turkey’s argument to drop the YPG.
“The entire world, for better or for worse from the Turkish point of view, is seeing [the YPG] as fighters, men and women, fighting against guys who are cutting people's heads off and making women sex slaves. The entire world is going to cheer when Raqqa falls,” says Mr. Aliriza.
“So Turkey’s ability to stop this process, and stop the support given to the YPG from across the board – not just the US, not just Russia – is going to be difficult,” he says.
While that may suit the Pentagon, by not delaying the Raqqa offensive, the risks for Turkey extend beyond Syria. Its battle with the PKK in southeast Turkey and northern Iraq has escalated for two years, and included high profile Kurdish bombings that have targeted Turkish security forces all the way to Ankara and Istanbul.
“If Turkey carries out more attacks into Syria, we will definitely see a rise in attacks in Turkey by the PKK against the Turkish Army … and we see for the first time the YPG responding to Turkish attacks,” says Güney Yildiz, a specialist on Turkey and Kurds, who has advised the British Parliament.
“The dichotomy is that if the US has to choose between Turkey and the YPG, they will definitely choose Turkey. But the question is whether they have to,” says Mr. Yildiz. “That’s a dichotomy pushed by Turkey or the Kurds, but what the Americans have been doing since autumn 2014 onwards is using both, and using both as leverage against each other.”
But how sustainable can that be, with the current trajectory of tension? Turkey’s noisy opposition to Kurdish gains in northern Syria first spilled over last August with Operation Euphrates Shield, a cross-border incursion that ostensibly sought to push ISIS back from Turkey’s border – but also aimed to prevent Kurdish forces from connecting individual cantons under their control into contiguous territory.
What happens when ISIS falls?
As the Raqqa offensive has neared, with US-backed Syrian Kurds ready to claim the prize, so have Turkey’s rhetoric and actions increased.
“It’s a very dangerous situation,” says Bonsey of ICG. But the longer-term problem for the YPG may be what happens in post-ISIS Syria, if the US moves its focus elsewhere.
While the YPG has proven to have “some very impressive tactical proficiency,” it may have also overestimated long-term US commitment, he says. “The YPG just does not seem to have a strategic answer for what to do, if and when that US role declines.”
Which leaves many wondering if Syria’s Kurds are being set up for the kind of betrayal that ethnic Kurds have been stung by repeatedly, for decades. Analysts note cases infamous among Kurds, such as the US selling them out to Iraq in 1975, when they believed the US guaranteed them aid from then-ally Iran.
They felt betrayed again by US military support for Saddam Hussein in the late 1980s, when the Iraqi dictator carried out a genocidal campaign against Kurds. And when President George H. W. Bush encouraged Kurds to rise up in 1991 – as Iraq’s Kurds remember it – the US allowed Mr. Hussein to crush the rebellion by not intervening to stop his helicopters and tanks.
“Kurdish history is littered with promises that were made to them,” says Aliriza from CSIS. But he doesn’t think it will necessarily happen again this time.
“I would argue that the level of engagement with the Syrian Kurds, because of its breadth and content, as well as its openness, is extraordinary,” says Aliriza. “This level of US military engagement is unprecedented.”

Hollywood casts a critical eye on tech visionaries
How do Silicon Valley execs see the world? Is it too rosy or too dystopian? In this next story, the Monitor’s Mike Farrell explores the mental models shaping technology and its use.

- Quick Read
- Deep Read ( 5 Min. )
Some of our keenest social observers are taking aim at a software-driven society. The film “The Circle,” along with shows like Netflix’s “Black Mirror” and HBO’s “Westworld,” represents a growing body of work meant to question how much power Silicon Valley industry visionaries have over our daily lives – and whether we want to go along for the ride. Often the problem with how Silicon Valley views the world, says Noam Cohen, author of the book “The Know-It-Alls,” is that, as he puts it, “everything is an engineering problem [to them].” Developers may perfect machines, he says. That doesn’t mean they should drive the culture. “Do we have to go there,” Mr. Cohen asks, “even if it’s not the best for all of us?”
Hollywood casts a critical eye on tech visionaries

The techno-exuberance on full display in “The Circle,” the movie adaptation of Dave Eggers’s 2013 book, is all too familiar for anyone who’s listened to Mark Zuckerberg or Elon Musk lately.
The founder of Facebook is on a mission to connect the entire planet “to amplify the good effects and mitigate the bad.” And the Tesla chief executive wants to colonize Mars.
It’s heady stuff. And it’s that kind of wide-eyed, shoot-for-the-stars (literally), disrupt everything, innovate-first-and-ask-questions-later attitude that “The Circle,” along with a growing body of films and TV shows, are questioning. Just how much power should the likes of Mr. Zuckerberg, Mr. Musk, and the other tech industry visionaries have over our daily lives? Where are they taking society? And do we want to go along for the ride?
“The Circle,” named for a fictional social media company that resembles a mash up of Apple, Facebook, and Google, is just Hollywood’s latest critique of a software-driven society. Remember the 1983 film “WarGames” and the computer that nearly destroyed civilization? And sci-fi films have long forecast dystopian futures in which computers threaten human survival – from HAL 9000 in "2001: A Space Odyssey" to Skynet in "The Terminator."
But now writers and directors are increasingly turning their attention to how technology affects more intimate and personal interactions: How we communicate, how we show affection, how we reveal our deepest thoughts and feelings, and whether personal privacy is a memento of the analog age.
In many ways, the growing body of work – in books, films, and television – critiquing Silicon Valley is about “the amount of power these companies have,” says Noam Cohen, a tech writer and author of the forthcoming book “The Know-It-Alls: The Rise of Silicon Valley as a Political Powerhouse and Social Wrecking Ball.” It’s a cultural response to their influence, he says.
Often the problem with how Silicon Valley views the world, he says, is that “everything is an engineering problem.” Developers may perfect a frictionless, real-time video platform or build a smarter robot he says, but that doesn’t mean society has to accept those machines, Mr. Cohen says. “Do we have to go there even if it’s not the best for all of us?”
Critique of technology, and its purveyors
For instance, the most recent season of Netflix’s “Black Mirror” offered a dark and unsettling critique of technology, beginning its third season last fall by portraying a life in which everyone is instantly judged by a social media score sheet. HBO’s “Westworld” imagines a future in which robots appear so human that real humans can’t differentiate between people and machines. And the most recent season of “Homeland,” the Showtime spy drama, included a subplot about an online fake news operation that was eerily similar to the Russian propaganda campaign ahead of the most recent presidential election.
One of the most stinging critiques of Silicon Valley comes from “Silicon Valley,” the HBO comedy from writer and director Mike Judge (who directed the films “Office Space” and “Idiocracy”). Last year, Andrew Marantz of The New Yorker called it the “first ambitious satire of any form to shed much light on the current socio-cultural moment in Northern California.”
“Silicon Valley” not only demystifies tech culture in ways that make it seem downright drab and often depicts the Northern California tech bubble in dark terms (making poignant statements about how tech companies and venture capital firms treat female engineers and immigrants).
The series is at its best when it's lampooning startup culture. Doree Shafrir's new novel "Startup" also takes jabs at the pretentiousness that's all too common among the young and brash tech workforce. She opens the books by describing a social media company's early morning dance party for its employees. "They posted this moment on Snapchat and Instagram, on Twitter and Facebook, anywhere that their message – I was here – could be loudly, clearly received."
Luddite's version of social media?
Neither the TV show nor the book paints nearly as a dark portrait about the overall internet economy as “The Circle,” directed by James Ponsoldt, who cowrote the movie with Eggers.
When Eggers’s book came out, it was panned by tech journalists as a luddite’s version of social media gone awry. In both book and movie, the social media company The Circle hatches an idea to spread tiny cameras around the world that can broadcast anything – at any time – via the web, a system that takes radical transparency (or radical surveillance) to an entirely new scale. And, in true Silicon Valley fashion, it launches the product, turns on the cameras, and waits to see what happens in the real world. Disruption in real time.
When The Circle’s leader Eamon Bailey (played by Tom Hanks) introduces the SeeChange camera system, he hails it as a mechanism for keeping tyrants and wrongdoers in check. “We will see it all; if it happens, we’ll know,” he says. “Imagine the human rights implications. The need to be accountable. So many of our lies that get us in trouble, the things we hide. We care about everybody you care about, because knowing is good. But knowing everything is better.”
That sort of wide-eyed optimism about technology without regard for any downsides (in this case, the complete end of privacy) isn't that dissimilar to the enthusiasm Zuckerberg showed for Facebook Live, the company's real-time video streaming platform. When it launched last year, he said it would offer users the “the most personal and emotional and raw and visceral ways ... to communicate.” But since then, amid the Chewbacca Moms and Martha Stewart videos, Facebook users have broadcast rapes, abuse, and even murders via Facebook Live. Facebook announced this week it was hiring 3,000 people to review posts and videos that might contain crimes or suicides.
To be sure, “The Circle,” which was widely panned, shows a one-dimensional view of Silicon Valley. It makes its point about privacy in blunt, Orwellian terms (the characters say things like “secrets are lies” and have a rather different take on the Care Bears slogan “sharing is caring”). However, critics say it fails to capture the full scope of how tech intermingles with society and how privacy (in some cases) can accompany a more interconnected world.
A Facebook employee who saw the film told The Guardian newspaper that the company’s employees are hardly “some homogeneous, dumbed-down, clap-for-everything crowd that’s like, ‘Yay! We hate privacy!’”
Other headline stories we’re watching
(Get live updates throughout the day.)The Monitor's View
Liberating students from a drinking culture
- Quick Read
- Deep Read ( 3 Min. )
-
By The Monitor's Editorial Board
The indictment of a Penn State fraternity after a student’s death from drinking should stir colleges to reframe the issue of alcohol use. The university’s reaction to this tragic case was, like that of many schools, simply punitive. Strategies aimed at scaring or deterring students have made only small improvements or have proved difficult to sustain. Students may respond less to fear and more to fulfilling opportunities. The best solution may lie in helping them cherish their ability to think clearly and to act responsibly toward themselves and others. Schools must show students how to live a good life, full of healthy relationships and learning – and free of the notion that liquor is a liberator.
Liberating students from a drinking culture

For more than two decades, college administrators, fearful of alcohol’s effects on young lives and learning, have tried many ways to curb excessive drinking by students. Those fears were revived last week when 18 members of a fraternity at Pennsylvania State University were criminally charged after a student died during a recent alcohol-laden initiation ceremony.
The remarkable indictments help highlight the need for a fresh approach to campus drinking, one based not just on fear of such student behavior but also on fulfilling the capacity of young people for healthy pursuits. The estimated 1,800 college students who die every year from alcohol-related injuries could have been guided toward safer ways to socialize or given better ways to overcome adolescent anxieties.
Penn State’s reaction to this tragic case was, like that of many schools, simply punitive. It cracked down on its fraternity system. And indeed, the indictment cites the school’s Greek community for “an environment so permissive of excessive drinking and hazing that it emboldened its members to repeatedly act with reckless disregard to human life.”
Yet in a signal for deeper thinking, Penn State President Eric Barron put out a plea: “For anyone looking across the national landscape, you realize that we have a national problem that is associated with excessive drinking.”
One way to reframe this issue is to take note of a recent survey by the University of Michigan. Among people ages 19 and 20, a quarter said they drink five or more drinks on a single occasion, or what’s called high-intensity drinking. That percentage jumps sharply for college students. The study’s chief author, Megan Patrick, explains the difference: “College attendance is associated with a freedom from adult responsibilities. Students, if they’re living with their parents, might not have the same opportunity to drink as students living on campus or in student housing.”
Ensuring that students are kept busy with an abundance of safe opportunities, from nonalcoholic parties to sports to volunteering, may be the better route for colleges and universities. Up to now, schools have relied mainly on negative messaging and stricter enforcement. Many offer – or even require – new students to view videos about the dangers of drinking, with the message that getting drunk is not a rite of passage. Some work with local liquor stores and restaurants to prevent underage drinking or purchases of alcohol. Others encourage students to act as “sober monitors” at social events where alcohol might be consumed. Last year, after the sexual assault of a student, Stanford University banned liquor from undergraduate parties.
Strategies aimed at scaring or deterring students, however, have made only small improvements or have proved difficult to sustain. Alumni, for example, often complain about new restrictions on the traditions of sororities and fraternities. Or schools are torn on whether to ban alcohol or introduce “safe” drinking habits.
The best solution may lie in helping students cherish their ability to think clearly and to act responsibly toward themselves and others. Simply operating out of a fear of drinking can be a tipsy tactic. Schools must show students how to live a good life, full of healthy relationships and learning – and free of the notion that liquor is a liberator.

A Christian Science Perspective
Each weekday, the Monitor includes one clearly labeled religious article offering spiritual insight on contemporary issues, including the news. The publication – in its various forms – is produced for anyone who cares about the progress of the human endeavor around the world and seeks news reported with compassion, intelligence, and an essentially constructive lens. For many, that caring has religious roots. For many, it does not. The Monitor has always embraced both audiences. The Monitor is owned by a church – The First Church of Christ, Scientist, in Boston – whose founder was concerned with both the state of the world and the quality of available news.
Getting past fear
- Quick Read
- Deep Read ( 5 Min. )
-
By Christopher Jones Contributor
Who hasn’t faced a situation that seemed unknown, troublesome, upsetting, or even frightful? We don't have to be held hostage by fear. The Bible relates in so many ways that we are actually made in the image of God. And so we can all express the certainty and stability that God includes.
Getting past fear
Several years ago, home alone one rainy Friday evening, I skimmed through my bookcase for a movie to keep me company. I chose one of my all-time favorites, an Alfred Hitchcock thriller. As I settled into watching it, I remembered how many times I'd seen this movie before, and yet I never tire of it. Although somewhat docile by today's cinematic standards, the first time I saw it as a boy I was so frightened I couldn’t get to sleep that night!
I know now that particular Hitchcock film isn't the only movie to instill this effect the first time someone watches it. Filmmakers purposely introduce elements of suspense, anticipation, surprise, fear, etc., which play on our emotions and make the initial impact of a film more intense and memorable. But, as is the case with many movies, once someone has seen the film and experienced its special effects, storyline twists, and surprise ending, the next time they watch it they are usually no longer afraid, anxious, worried, etc., because the mystery has been dispelled.
I have found this analogy so helpful in dealing with the many challenges I've encountered in my life. Who among us hasn't faced a situation that seemed unknown, troublesome, upsetting, frightful, or even evil? Hardly a day or a week goes by without some experience popping up where we cannot predict or control the outcome. In such a case, there is often a temptation to react much as we might to a new movie – with fear, shock, excitement, anxiety, stress, worry, mistrust, and so on.
A friend once described worry as "the lowest form of thought." Worry presupposes either a separation from God or His impotence. Through worry, we relinquish our claim to a sure, orderly, and beneficent universe, and plunge ourselves into a world of chaotic and conflicting forces, where evil and good must constantly battle to determine which shall prevail in any given circumstance. It is a desperate state of mind in which we are never comfortable and which often impels us to feel personally responsible for the outcome of a situation.
But we don't have to be held hostage by these thoughts. Instead, we can know that, as the Bible tells us in so many ways, we are actually made and maintained in the image of God – as the harmonious, good, truthful, and confident reflection of our omnipresent and omnipotent Father-Mother – and thus reflect all the stability, certainty, and harmony that God includes. This awareness lets us deal with daily trials much as we would with a movie we've previously seen.
We already know the outcome and it can only be one thing – good! Yielding our thought to God and putting all our trust in Him, we discern that this divine Principle will never – could never – let us down, and we can lead our lives feeling certain that every challenge, interaction, and opportunity will not only resolve itself harmoniously, but will end up blessing us and lifting us up to new spiritual heights. With God as our Director, we can know that the myriad dramas of our life will always result in a happy resolution, guaranteed!
Mary Baker Eddy, the founder of Christian Science, wrote in "Science and Health with Key to the Scriptures" : "When we wait patiently on God and seek Truth righteously, He directs our path" (p. 254). Sometimes we might think that waiting patiently and seeking are contradictory activities, but if we think of waiting as an active state of thought, full of anticipation, receptivity, and joy, we begin to see how our pursuit for Truth can be filled with patience, expectancy, hope, assurance.
I saw this most vividly in an experience about a year ago. I had stopped at the Post Office to get my mail on the way to picking up my son at school. As I quickly shuffled through the letters, one from the Internal Revenue Service caught my eye. I hurriedly scanned it to discover that in auditing my 2008 tax return, the IRS was not able to substantiate a number of deductions I had claimed that year. The letter went on to say that if I wasn't able to produce documentation for these deductions within 30 days, they would be disallowing them and sending me a tax bill – for back taxes and penalties – amounting to more than $100,000!
I was panic-stricken. As I walked back to my car all sorts of thoughts swirled through my head: How could I have made such a major mistake on my tax return? Will the IRS let me pay off this huge debt over time? If not, maybe I could take out a second mortgage on our home.
Fortunately, the 15-minute drive to my son's school gave me time to calm down and collect my thoughts. One of the first things that came to me was a passage from Jeremiah, "I know the thoughts that I think toward you, saith the Lord, thoughts of peace, and not of evil, to give you an expected end" (29:11). I realized that an "expected end" wasn't necessarily knowing exactly how this calamity would be resolved, but knowing that if I let God handle it completely, I wouldn't need to worry about it – I could expect the ending to be perfect and good.
By the time I picked up my son, I had turned the whole problem over to God in my thought. I became peaceful about it, as well as alert to what God was telling me to do next. The following day I was led to call the man who'd helped me prepare my 2008 tax return. Over the next several days we were able to gather and resubmit all the necessary documentation. Within a few months we received confirmation from the IRS that they were satisfied with our submittal and the case was now closed.
While I was grateful for this small example of God's care and sureness, what can we do when we've prayed about a situation which didn't seem to have a happy resolution? Perhaps a loved one passed away, a spouse left us, or we learned of terrible suffering from a natural disaster. By holding fast to God's immortal, absolute ideas, we deepen our appreciation of the reliability and unchangeableness of the universe that includes us. We pierce the material haze surrounding what seems to be happening in our world, and perceive the spiritual reality behind it. True, it may not be the endings we imagine, but if we listen earnestly and openly to God, we will find that His solutions are always brimming with love, perfection, and goodness, which dispel our grief and uncertainty, and naturally bless us.
Each opportunity we have to demonstrate that life isn't a giant mystery, but rather that God is always in complete control of every situation, is another solid step forward on our spiritual path, and better equips us to handle the next challenge. Like watching a movie for the second time, all the mystery and uncertainty vanish, replaced by the joyful expectancy and assurance that we can never be separated from God, are always in His thoughts, and can rely wholeheartedly on His tender, loving care.
This article was adapted from an article in the April 13, 2011, issue of the Christian Science Sentinel.

A message of love
Dissent that crosses borders

A look ahead
Thank you for reading today.
A quick note: If you listened to the audio version yesterday, then you heard about a video to accompany our story about the stewardship of Western public lands. We do have the video – but we didn’t add it to the story in time. If you want to view it now, please hit the back-issue arrow next to “more issues” below. Thanks for bearing with us.
Tomorrow, in Part 2 of today’s special report, we’ll look at how mothers of drug addicts are creating an informal network to help others avoid the pitfalls they experienced.




