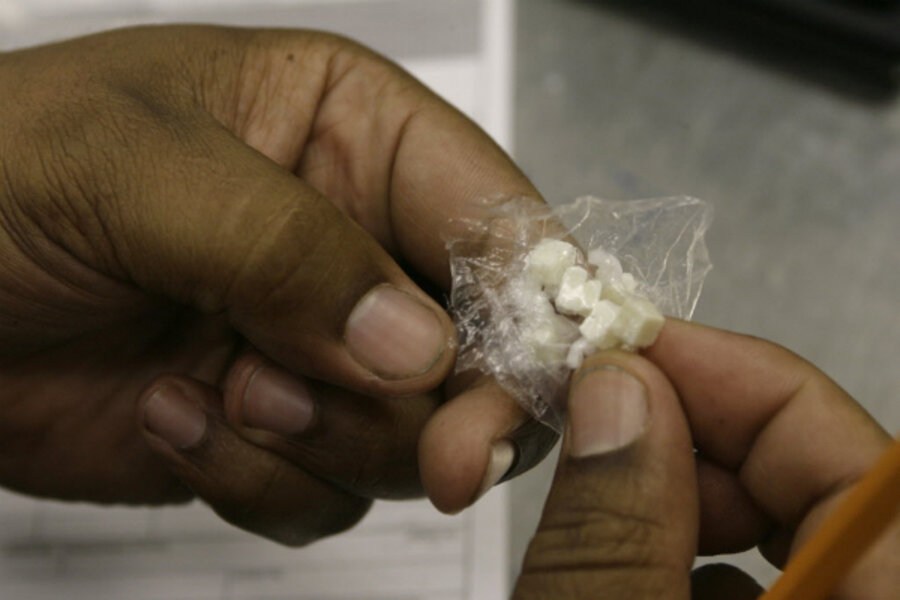
'Crack baby' development issues not side-effect of drug, but poverty
Loading...
Jaimee Drakewood hurried in from the rain, eager to get to her final appointment at Children's Hospital of Philadelphia.
Ever since her birth 23 years ago, a team of researchers has been tracking every aspect of her development — gauging her progress as an infant, measuring her IQ as a preschooler, even peering into her adolescent brain using an MRI machine.
Now, after nearly a quarter century, the federally funded study was ending, and the question the researchers had been asking was answered.
Did cocaine harm the long-term development of children like Jaimee, who were exposed to the drug in their mother's womb?
The researchers had expected the answer would be a resounding yes. But it wasn't. Another factor would prove far more critical.
___
A crack epidemic was raging in Philadelphia in 1989 when Hallam Hurt, then chair of neonatology at Albert Einstein Medical Center on North Broad Street, began a study to evaluate the effects of in-utero cocaine exposure on babies.
In maternity wards in Philadelphia and elsewhere, caregivers were seeing more mothers hooked on cheap, smokable crackcocaine. A 1989 study in Philadelphia found that nearly one in six newborns at city hospitals had mothers who tested positive for cocaine.
Troubling stories were circulating about the so-called crack babies. They had small heads and were easily agitated, according to reports, many of which were anecdotal. The babies also seemed aloof and avoided eye contact.
Some social workers predicted a lost generation — kids with a host of learning and emotional deficits who would overwhelm school systems and not be able to hold a job or form meaningful relationships. The "crack baby" image became symbolic of bad mothering, and some cocaine-using mothers had their babies taken from them or, in a few cases, were arrested.
It was amid that climate that Hurt organized a study of 224 near-term or full-term babies born at Einstein between 1989 and 1992 — half with mothers who used cocaine during pregnancy and half who were not exposed to the drug in utero. All the babies came from low-income families, and nearly all were African-Americans.
Hurt hoped the study would inform doctors and nurses caring for cocaine-exposed babies and even guide policies for drug prevention, treatment, and follow-up interventions. But she never anticipated that the study, funded by the National Institute on Drug Abuse, would become one of the largest and longest-running studies of in-utero cocaine exposure.
One mother who signed up was Jaimee's mom, Karen Drakewood. She was on an all-night crack binge in a drug house near her home in the city's West Oak Lane section when she went into labor. Jaimee was born Jan. 13, 1990, weighing an even 7 pounds.
"Jaimee was beautiful when she was born. A head full of hair. She looked like a porcelain doll," Karen Drakewood, now 51, said recently in her Overbrook kitchen. "She was perfect."
But Drakewood knew looks could be deceiving.
"My worst fear was that Jaimee would be slow, mentally retarded, or something like that because of me doing drugs," she said. She agreed to enroll her baby in the cocaine study at Einstein.
Drakewood promised herself that she would turn her life around for the sake of Jaimee and her older daughter, but she soon went back to smoking crack.
___
Hurt arrived early at Children's Hospital one morning in June to give a talk on her team's findings to co-workers.
After nearly 25 years of studying the effects of cocaine and publishing or presenting dozens of findings, it wasn't easy to summarize it in a PowerPoint presentation. The study received nearly $7.9 million in federal funding over the years, as well as $130,000 from the Einstein Society.
Hurt, who had taken her team from Einstein to Children's in 2003, began her lecture with quotations from the media around the time the study began. A social worker on TV predicted that a crack baby would grow up to "have an IQ of perhaps 50."
A print article quoted a psychologist as saying "crack was interfering with the central core of what it is to be human," and yet another article predicted that crack babies were "doomed to a life of uncertain suffering, of probable deviance, of permanent inferiority."
Hurt, who is also a professor of pediatrics at the University of Pennsylvania, is always quick to point out that cocaine can have devastating effects on pregnancy. The drug can, for instance, cause a problematic rise in a pregnant woman's blood pressure and trigger premature labor.
Babies born prematurely, no matter the cause, are at risk for a host of medical and developmental problems. On top of that, a parent's drug use can create a chaotic home life for a child.
Hurt's study enrolled only full-term babies so the possible effects of prematurity did not skew the results. The babies were then evaluated periodically, beginning at six months and then every six or 12 months on through young adulthood. Their mothers agreed to be tested for drug use throughout the study.
The researchers consistently found no significant differences between the cocaine-exposed children and the controls. At age 4, for instance, the average IQ of the cocaine-exposed children was 79.0 and the average IQ for the non-exposed children was 81.9. Both numbers are well below the average of 90 to 109 for U.S. children in the same age group.
When it came to school readiness at age 6, about 25 percent of children in each group scored in the abnormal range on tests for math and letter and word recognition.
"We went looking for the effects of cocaine," Hurt said. But after a time "we began to ask, 'Was there something else going on?'"
While the cocaine-exposed children and a group of non-exposed controls performed about the same on tests, both groups lagged on developmental and intellectual measures compared to the norm. Hurt and her team began to think the "something else" was poverty.
As the children grew, the researchers did many evaluations to tease out environmental factors that could be affecting their development. On the upside, they found that children being raised in a nurturing home — measured by such factors as caregiver warmth and affection and language stimulation - were doing better than kids in a less nurturing home.
On the downside, they found that 81 percent of the children had seen someone arrested; 74 percent had heard gunshots; 35 percent had seen someone get shot; and 19 percent had seen a dead body outside — and the kids were only 7 years old at the time. Those children who reported a high exposure to violence were likelier to show signs of depression and anxiety and to have lower self-esteem.
More recently, the team did MRI scans on the participants' brains.
The investigators found one brain area linked to attention skills that differed between exposed and non-exposed children, but they could not find any clinically significant effect on behavioral tests of attention skills. Drug use did not differ between the exposed and non-exposed participants as young adults.
About 42 percent used marijuana and three tested positive for cocaine one time each. The team has kept tabs on 110 of the 224 children originally in the study. Of the 110, two are dead — one shot in a bar and another in a drive-by shooting — three are in prison, six graduated from college, and six more are on track to graduate. There have been 60 children born to the 110 participants. The years of tracking kids have led Hurt to a conclusion she didn't see coming.
"Poverty is a more powerful influence on the outcome of inner-city children than gestational exposure to cocaine," Hurt said at her May lecture.
Other researchers also couldn't find any devastating effects from cocaine exposure in the womb.
Claire Coles, a psychiatry professor at Emory University, has been tracking a group of low-income Atlanta children. Her work has found that cocaine exposure does not seem to affect children's overall cognition and school performance, but some evidence suggests that these children are less able to regulate their reactions to stressful stimuli, which could affect learning and emotional health. Coles said her research had found nothing to back up predictions that cocaine-exposed babies were doomed for life.
"As a society we say, 'Cocaine is bad and therefore it must cause damage to babies,'" Coles said. "When you have a myth, it tends to linger for a long time."
Deborah A. Frank, a pediatrics professor at Boston University who has tracked a similar group of children, said the "crack baby" label led to erroneous stereotyping.
"You can't walk into a classroom and tell this kid was exposed and this kid was not," Frank said. "Unfortunately, there are so many factors that affect poor kids. They have to deal with so much stress and deprivation. We have also found that exposure to violence is a huge factor."
Frank said that cocaine — along with other illicit drugs, alcohol, and cigarettes — "isn't good for babies," but the belief that they would "grow up to be addicts and criminals is not true. Some kids have stunned us with how well they've done."
___
Jaimee Drakewood came to her last visit at Children's with her 16-month-old son KyMani in tow.
It was the 31st time she had met with the researchers.
"We do appreciate everything you've done, because it's not easy to get to all these appointments," said team member Kathleen Dooley, as she handed Drakewood a framed certificate of appreciation. "We are proud of you and we feel you are family, because you are."
The team plans to stay in touch with study participants each year. They have started a new study that uses MRI and other tools to explore the neural and cognitive effects of poverty on infant development.
"Given what we learned," Hurt said, "we are invested in better understanding the effects of poverty. How can early effects be detected? Which developing systems are affected? And most important, how can findings inform interventions for our children?"
The team considers Jaimee and her mother, Karen, among their best success stories. Jaimee is heading into her senior year at Tuskegee University in Alabama and hopes to become a food inspector. She is home for the summer with her son and working as a lifeguard at a city pool.
After a few starts and stops, including a year in jail, Karen Drakewood is off drugs and works as a residential adviser at Gaudenzia House. Her older daughter just received a master's degree at Drexel University; her son is a student at Florida Atlantic University.
Even in the worst moments, Karen Drakewood said she tried to show her kids "what their future could hold." ''If a child sees the light, they will follow it." Jaimee Drakewood credits her big sister and mother for keeping her on track.
"I've seen my mom at her lowest point and I've seen her at her highest. That hasn't stopped me from seeing the superwoman in her regardless of where she was at," Jaimee said.
Despite her family's history, Jaimee believes she and her siblings are "destined to have accomplishments, to be greater than our parents."